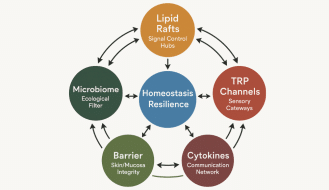
How Your Gut Health Influences Your Immune System
Experts saw this pandemic coming.
Already in the 1990s – and throughout the last two decades – scientists repeatedly warned us about the increasing likelihood of global pandemics due to globalization, urbanization, and more (1, 2).
Now that COVID-19 has arrived, many efforts feel like too little, too late. But there are still things that we can do to mitigate damage. One of them includes mobilizing “specialized forces” that are key to resisting, surviving, and recovering from infections.
I am talking about the microbiome.
How Does Gut Health Affect the Immune System?
One of the most astounding recent developments in medicine is the notion that our gut bacteria (also commonly referred to as the microbiome) control our immune system and susceptibility to chronic illnesses, like diabetes, cardiovascular disease, and certain types of cancers (3).
But the microbiome also influences our vulnerability to infection.
Starting from birth, our gut bacteria develop a fascinating collaboration with our immune cells. When harmful pathogens make their way into our digestive system, our gut bacteria are at the frontlines. They combat these pathogenic bacteria and viruses by competing with them for nutrients and adhesion sites, releasing toxins to prevent these bad actors from taking hold, and by signaling our immune cells into action (4).
Around 70-80% of our immune cells are located in the gut, stressing the importance of their collaboration with the gut microbiome (5).
What Is Dysbiosis?
Because of this relationship between the immune cells and our microbiome, it’s critical to foster a varied, healthy composition of bacteria throughout life. It comes as no surprise that dysbiosis – or having a poor microbial balance – is linked to most illnesses and health outcomes (6).
The two highest risk factors for dying from infections are advanced age and having a pre-existing, poorly controlled chronic illness. In both of these scenarios, dysbiosis plays a role (7, 8).
Dysbiosis occurs when the composition of our resident bacteria becomes unbalanced – either through a loss of beneficial bacteria, the overgrowth of harmful bacteria, and/or the loss of microbial diversity.
How to Improve Our Gut Health
While we can’t change our age, we can certainly work to improve the health of our gut bacteria through a variety of means:
Eating a Balanced Diet
There is an old saying that we are what we eat. And if you consider what diet does to the microbiome, this makes sense: We harbor the types of bacteria that favor our food and lifestyle.
Western diets – which are typically low in fiber and saturated with refined sugars and the wrong kinds of fats – are especially appreciated by bacteria that send out inflammation-stimulating and intestinal-wall destroying substances (9). When we consume these kinds of diets, it nourishes the overgrowth of these inflammation-driving bacteria at the expense of our ally microbes.
The consequence is that the immune system is already over-challenged and worn out, with little ability to fight new infections from pathogenic viruses or bacteria.
Why Nutrition Matters
Poor nutrition status is almost always linked to poor health outcomes for any disease. While history has repeatedly acknowledged the importance of getting the right nutrients, it is disheartening that we have developed a society that frequently undermines this fact. Even in hospitals, where people are most at risk and need the highest quality diet, patients are typically offered poor-quality foods that are loaded with pro-inflammatory oils and high levels of refined sugars (10).
Numerous studies are now exploring the role of probiotics for restoring a healthy microbiome. But perhaps most important of all is increasing our intake of beneficial fibers from whole foods like oats, nuts, lentils, beans, fruits, and vegetables.
As we’ve discussed in previous articles, having a healthy intake of omega-3s is also important for maintaining a good balance of gut bacteria.

Eating a Mediterranean Diet rich in whole foods filled with fibers and omega-3s is one of the best ways to maintain a healthy microbiome.
Having a Healthier Lifestyle
The health of our microbiome is not just diet-dependent. Lifestyle factors – like exercise and exposure to sunshine (the primary producer of vitamin D3) – also have positive microbiome-regulating abilities (11). For instance, studies in humans and mice show that aerobic exercise can increase microbial diversity in the gut (12).
On the flip side, behaviors like smoking, drinking alcohol, and unnecessary antibiotic use are associated with poor microbial health (13, 14). An estimated 30% of antibiotics given to children are not medically necessary. This is especially disturbing since antibiotic misuse can have long-term negative effects on the microbiome and immune system (15, 16).
Getting Enough Sleep
The impact of sleep on the microbiome is something that does not get enough attention. Studies reveal that changes in our sleep pattern (as well as sleep deprivation) can disturb the diversity and composition of our microbiome. This connection could partly explain why health care workers who work night shifts are more susceptible to respiratory infections than those who do not work during the night (17, 18).
Mice studies indicate that melatonin supplementation also increases microbial diversity and promotes a healthier balance of gut bacteria (18). This connection has led scientists to theorize that the beneficial effects of melatonin may be partially due to this molecule’s microbiome-regulating abilities. After all, just like our human cells, our gut bacteria also carry out their roles in the body in response to the circadian rhythm.

Produced in the pineal gland in response to darkness, melatonin controls our circadian rhythm and signals to the body when it is time to sleep.
The Best Ways to Protect Your Microbiome
As unpleasant as the thought is, COVID-19 may not be the last pandemic we will witness in our lifetimes. In fact, experts believe that global viral outbreaks may become more prevalent in coming years (19).
Governments worldwide need to respond accordingly: It’s not just a matter of combatting the COVID-19 crisis now, but also thinking ahead for the future.
As individuals, we can also prepare by establishing good habits that will serve us now and for whatever lies ahead:
1. Wash our hands correctly and frequently.
2. Be aware that having an infection puts other people at risk and change our behavior accordingly.
3. Reduce our consumption of processed foods and opt for a Mediterranean diet full of fibers, fruits, vegetables, nuts and enough omega-3s every day.
4. Exercise regularly.
5. Practice good sleep hygiene by keeping a consistent bedtime, lowering the bedroom temperature, and removing electronics from the bedroom. Remember that even short-term exposure to light at night will disrupt melatonin secretion in the brain.
6. Get some sunshine. This will not only boost the vitamin D3 content in your body (which stimulates its microbe-fighting abilities), but also improve melatonin production at night (20, 21).
7. Focus on the things in life that bring you joy. For me, that includes getting a good night’s rest, reading, phone calls with family and friends, walking around the neighborhood with my wife.
Good luck to us all!
For More Restful Sleep and Energy
Experience the Omega3 Innovations difference for yourself with the most effective fish oil supplement on the market.
Buy Now
References:
1. Madhav, N., Oppenheim, B., Gallivan, M., et al. (2017). Pandemics: Risks, Impacts, and Mitigation. Disease Control Priorities: Improving Health and Reducing Poverty, 3rd Edition. International Bank for Reconstruction and Development / The World Bank.
2. McVeigh, K. (2019, September). Experts Warn World ‘Grossly Unprepared’ for Future Pandemics. The Guardian.
3. Wang, B., Yao, M., Lv, L., Ling, Z., & Li, L. (2017). The Human Microbiota in Health and Disease. Engineering, 3 (1): 71 – 82.
4. Veronica, L., Lia-Mara, D., Gradisteanu, P. G., et al. (2018). Aspects of Gut Microbiota and Immune System Interactions in Infectious Diseases, Immunopathology, and Cancer. Frontiers in Immunology, 9: 1830.
5. Adaes, S. (2019, July). How the Gut Microbiota Influences Our Immune System. Neurohacker Collective.
6. DeGruttola, A. K., Low, D., Mizoguchi, A., & Mizoguchi, E. (2016). Current Understanding of Dysbiosis in Disease in Human and Animal Models. Inflammatory Bowel Diseases, 22(5), 1137–1150.
7. Cianci, R., Pagliari, D., Piccirillo, C. A., Fritz, J. H., & Gambassi, G. (2018). The Microbiota and Immune System Crosstalk in Health and Disease. Mediators of Inflammation, 2018, 2912539.
8. Nagpal, R., Mainali, R., Ahmadi, S., et al. (2018). Gut Microbiome and Aging: Physiological and Mechanistic Insights. Nutrition and Healthy Aging, 4(4), 267–285.
9. Lobionda, S., Sittipo, P., Kwon, H. Y., & Lee, Y. K. (2019). The Role of Gut Microbiota in Intestinal Inflammation with Respect to Diet and Extrinsic Stressors. Microorganisms, 7(8), 271.
10. McCluskey, M. (2020, March). Healthy Eating Is Key To Well-Being. So Why Is Hospital Food Often So Bad? The Huffington Post.
11. (2019, October). Exposure to Sunlight Boosts Good Gut Microbiome Bacteria, and Vitamin D Levels. Genetic Engineer and Biotechnology News.
12. Dalton, A., Mermier, C., & Zuhl, M. (2019). Exercise Influence on the Microbiome-Gut-Brain Axis. Gut Microbes, 10(5), 555–568.
13. Hills, R. D., Jr, Pontefract, B. A., Mishcon, H. R., Black, C. A., Sutton, S. C., & Theberge, C. R. (2019). Gut Microbiome: Profound Implications for Diet and Disease. Nutrients, 11(7), 1613.
14. Conlon, M. A., & Bird, A. R. (2014). The Impact of Diet and Lifestyle on Gut Microbiota and Human Health. Nutrients, 7(1), 17–44.
15. Antibiotic Use in Outpatient Settings, 2017. Centers for Disease Control and Prevention.
16. Vangay, P., Ward, T., Gerber, J. S., & Knights, D. (2015). Antibiotics, Pediatric Dysbiosis, and Disease. Cell Host & Microbe, 17(5), 553–564.
17. Li, Y., Hao, Y., Fan, F., & Zhang, B. (2018). The Role of Microbiome in Insomnia, Circadian Disturbance and Depression. Frontiers in Psychiatry, 9, 669.
18. Loef, B., Van Baarle, D., Van Der Beek, A. J., Sanders, E. A., Bruijning-Verhagen, P., Proper, K. I. (2019). Shift Work and Respiratory Infections in Health-Care Workers. American Journal of Epidemiology, 188(3): 509–517.
19. Hilsenrath, J. (2020, March). Global Viral Outbreaks Like Coronavirus, Once Rare, Will Become More Common. The Wall Street Journal.
20. Parkar, S. G., Kalsbeek, A., & Cheeseman, J. F. (2019). Potential Role for the Gut Microbiota in Modulating Host Circadian Rhythms and Metabolic Health. Microorganisms, 7(2), 41.
21. Mead M. N. (2008). Benefits of Sunlight: A Bright Spot for Human Health. Environmental Health Perspectives, 116(4), A160–A167.
Popular posts


Related posts