Melatonin & COVID-19: Can This ‘Sleep Hormone’ Help?
It started with a runny nose and a slight cough. But when his 72-year-old wife tested positive for COVID-19, he got concerned.
“Is there any research suggesting the supplements we are taking might help?” he called our office to ask. He had read several of our blogs on the immune roles of omega-3s and vitamin D3.
“Actually,” I told him, “the most interesting nutrient might be melatonin.”
Does Melatonin Help Your Immune System?
Melatonin’s role in immune health might come as a surprise to many. Most people still think of melatonin as a sleep aid. This humble “sleep hormone,” however, has anti-inflammatory and antioxidant effects that are relevant for fighting many diseases.
With regards to COVID-19, over 140 scientific articles to date have recommended melatonin be considered a “safe and potentially effective” treatment (1). One recent trial even found that melatonin was at least 2X as effective as the drugs Remdesivir and Tocilizumab for reducing COVID-19 inflammatory markers (1, 2).
So how exactly does melatonin impact our immune system? And how does melatonin perform in COVID-19 trials? Let’s take a closer look!
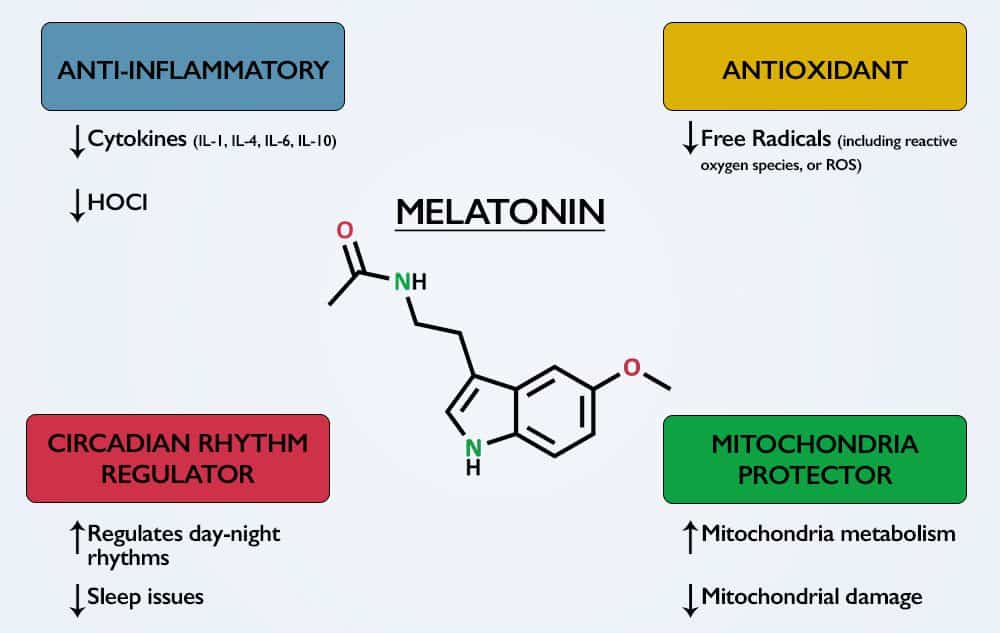
Misunderstood melatonin: Melatonin’s benefits extend far beyond sleep.
Melatonin Curbs Excessive Inflammation
When we get sick, our bodies respond by recruiting lots of inflammatory molecules. Inflammation (manifesting as redness, swelling, pain, and loss of function) is a normal biological process meant to kill off the invading pathogen.
Inflammation doesn’t come for free, however. In the same process, the body produces reactive oxygen species, or ROS. Too much ROS can be dangerous, leading to cell death and organ damage.
That’s where melatonin comes in. As an antioxidant, melatonin helps clean up excessive ROS. It also keeps inflammatory molecules from over-producing. These include:
Cytokines – The Bringers of the ‘Cytokine Storm’
Before COVID-19, only rheumatologists and immunologists were concerned about cytokines. Today, after several years of living through the pandemic, most people have heard about the dreaded ‘cytokine storm.’ Essentially, if too many cytokines are released into the bloodstream at once, they create havoc. As noted in many news reports, a cytokine storm can cause multiple-organ failure.
Melatonin downregulates several inflammatory cytokines, including interleukin-6 (2). That’s why melatonin has been shown in a variety of disease contexts to fight cytokine storms (1).
MPO – An Enzyme that Pumps Up Oxidative Stress
In response to COVID-19, white blood cells release an enzyme called myeloperoxidase (MPO). Like a chemical crowbar, MPO pries open a substance called hypochlorous acid, or HOCl. When too much HOCI is released, it can cause tissue damage and lead to conditions like acute lung injury. As a result, the lungs don’t manage to make use of oxygen, despite being on a respirator (3).
Melatonin is a potent MPO inhibitor (3). By keeping MPO and HOCI at bay, melatonin prevents inflammation from getting out of hand and destroying the body.
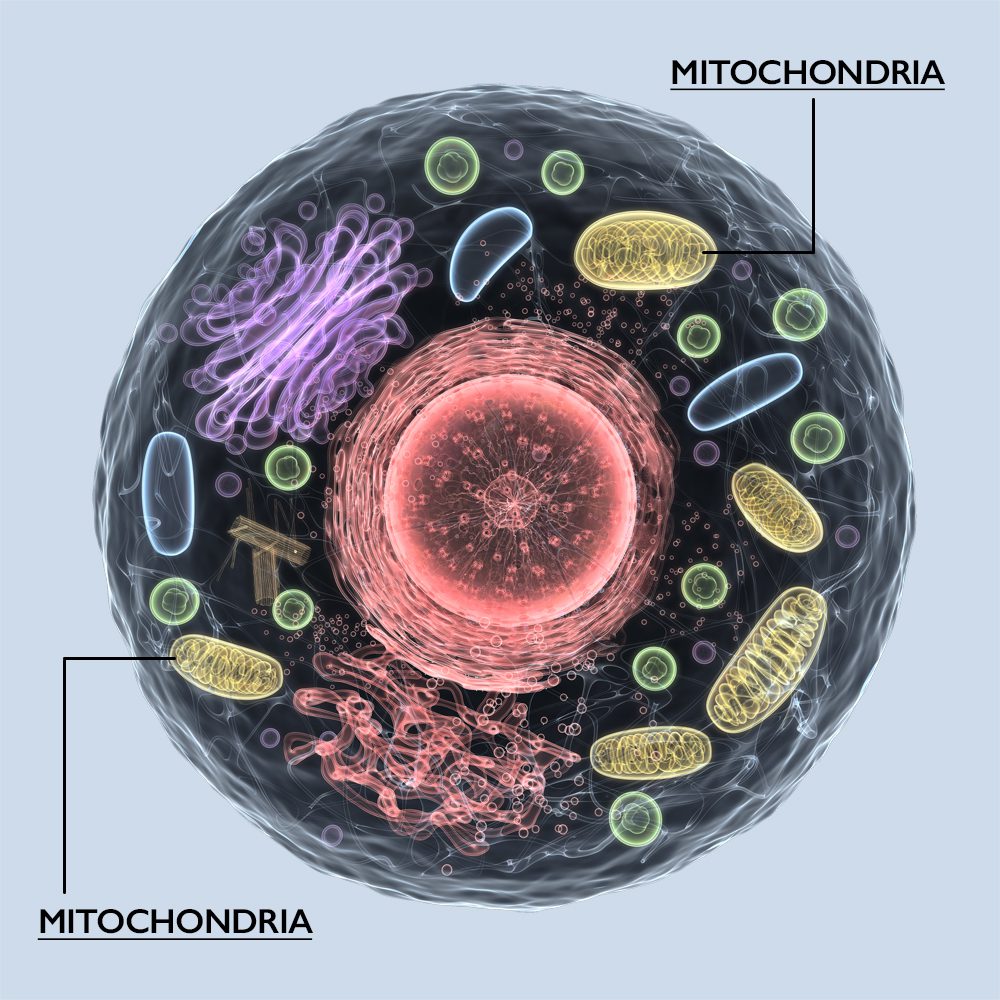
Beyond the brain: Melatonin is produced in the brain’s pineal gland at night. It’s also made in the mitochondria of every cell in your body!
Melatonin Keeps the Mitochondria Healthy
The mitochondria are the power stations of the cell. These organelles make the cell’s energy, maintain cell immunity and homeostasis, and determine cell survival or death.
It’s thought that SARS-CoV-2 “hijacks” the immune cells’ mitochondria to replicate and spread. This mitochondrial disruption can trigger cell death with all of its consequences. For instance, too much mitochondrial damage in heart cells can lead to heart failure and cardiac arrest (4).
Melatonin is produced in the mitochondria of all organs (3). One of its prime functions there is to clean up harmful molecules called free radicals, which are created in the energy-making process. Melatonin also improves mitochondrial biogenesis, which is the process by which the cells make more mitochondria (5). That’s important, since mitochondrial biogenesis is associated with anti-aging and fewer diseases.
Long story short, melatonin protects the mitochondria and keeps these vital cell structures functioning as they should. This in turn means the body is better able to fight off invading viruses.
Melatonin Regulates Our Circadian Rhythm
The circadian rhythm, or our “internal clock,” drives many of our immune responses. For example, the body produces more anti-inflammatory mediators when we sleep at night, and good sleep is linked with a better vaccine response (6).
When our circadian rhythm is disrupted, our immune health suffers. Plus, the level of inflammation in our body increases. It’s no surprise then that studies associate sleep loss with an increase in infections and severe disease (6). This holds true for COVID-19, too.
Melatonin is one of the body’s most important circadian rhythm regulators. Unfortunately though, many people have low melatonin levels, due to aging, prior disease, or exposure to light at night. When a person fails to get enough melatonin, their circadian rhythm gets off kilter. They struggle to fall asleep, wake up frequently, and have poor quality rest.
Numerous scientific reviews have suggested that melatonin supplementation may restore the circadian rhythm of COVID-19 patients (7). Indeed, one study found that melatonin increased the amount of sleep and reduced the number of delirium episodes of hospitalized patients (8).
What the science says: Melatonin studies on COVID-19 patients have, by and large, found very promising results.
How Has Melatonin Performed in COVID-19 Trials?
Melatonin has a good track record when it comes to viral infections. In past studies, researchers have found that melatonin reduced the severity and risk of death from other types of viruses, including three different types of coronaviruses (1).
When COVID-19 first came on the scene, some scientists recommended using melatonin based on the strength of this data alone. Today, however, more studies have been able to document melatonin’s effects on COVID-19 directly. Here is what they have found:
• A meta-analysis of 3 placebo-controlled trials found that patients on melatonin had a higher recovery rate. The melatonin group also had a lower risk of being admitted to the ICU and dying compared to the control group (9).
• A retrospective analysis of 791 intubated patients found that those treated with melatonin had a “markedly lower risk” of dying (10).
• A retrospective study of 2463 hospitalized patients found that those given melatonin had a lower mortality rate compared to the non-melatonin group (11).
• Two randomized prospective studies linked melatonin with a reduction in sepsis and COVID-19 symptoms. A third found that melatonin increased blood oxygen and sleep time (both important for recovery) (1).
• In a study of mild to moderate COVID-19 patients, those taking 10 mg of melatonin recovered faster and scored higher on a quality of life survey. This was compared to patients receiving placebo or vitamin C (12).
Not all studies have found such glowing results. Two other retrospective studies did not find that melatonin supplementation lowered the mortality rate of hospitalized patients (13, 14).
Why the discrepancy? All of the studies noted above used different melatonin dosages and examined different types of patient groups. Since the conditions were not the same, it makes sense that the results vary.
How Much Melatonin for COVD-19?
One of the biggest questions about melatonin is the dose necessary to get good results. Unfortunately, science has yet to provide a one-size-fits-all answer. In COVID-19 trials, scientists have used doses ranging from 3 mg – 600 mg daily (1)!
Some scientists suspect that the optimal melatonin dose may depend on age. That’s because older people often have significantly reduced melatonin levels from the outset (1). A person’s body weight and disease severity might also influence the best dose.
Brusco et al speculated that 9 mg of melatonin per day might be enough to help patients reduce their stay in the ICU (5). Another therapeutic algorithm suggested 3 – 10 mg daily for elderly people with medical comorbidities as a protective measure (5, 15).
While more studies on dose are needed to clarify the dose question, no trials have found any toxicity related to melatonin. This includes the studies using the highest dosages.
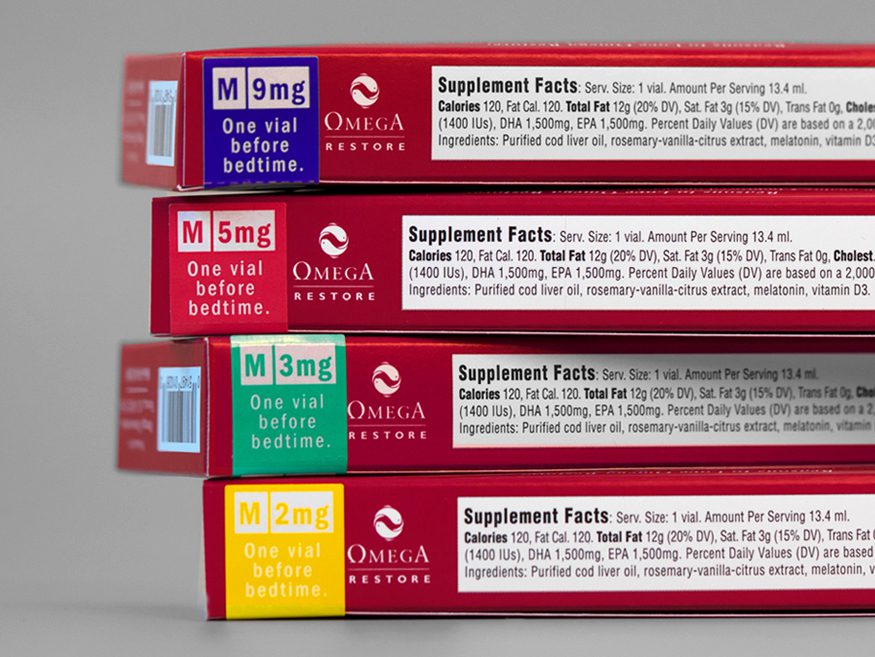
How many milligrams? Researchers are still working to determine the best melatonin dose for COVID-19 patients. Likely, the answer will vary somewhat depending on the individual.
Why Omega-3 + Vitamin D + Melatonin?
Melatonin indisputably plays many roles in our immune health. But this fascinating molecule may be even more effective when it’s coupled with other treatments and nutrients.
Here at Omega3 Innovations, we are most interested in the relationship between melatonin, omega-3s and vitamin D. Melatonin, omega-3s and vitamin D have complementary anti-inflammatory properties. These nutrients are all important for curbing the excessive inflammation that can lead to a cytokine storm and other nasty COVID-19 complications. Melatonin and vitamin D also share complementary antioxidant and immune-modulatory effects (16).
Besides working synergistically, these nutrients depend on each other. For example, omega-3s may increase the production of melatonin in our bodies (17). In return, melatonin works as an antioxidant to protect the integrity and function of the omega-3s.
To better understand the relationship between the three, think about a computer. Omega-3s are like the hardware of the cell, helping ensure the integrity and proper functioning of the cell membrane. The vitamin D receptors and the melatonin are like the software that send signals to other parts of the body. All three have to be in place for the cell to function well.
Melatonin Matters for COVID-19 & More
The rapid rate at which SARS-CoV-2 mutates makes it difficult to keep up with vaccines. And while we thankfully have better treatments for COVID-19 today than we did at the start of the pandemic, experts agree we still need more.
The good news is, even while the virus mutates, melatonin’s ability to fight inflammation, regulate our circadian rhythm, and protect the mitochondria remains the same. That’s why this powerful nutrient will continue to be relevant for not just COVID-19, but whatever immune challenges come our way.
For More Restful Sleep and Energy
Experience the Omega3 Innovations difference for yourself with the most effective fish oil supplement on the market.
Buy Now
References:
1. Reiter, R. J., Sharma, R., Simko, F., Dominguez-Rodriguez, A. et al. (2022). Melatonin: Highlighting Its Use as a Potential Treatment for SARS-CoV-2 Infection. Cellular and Molecular Life Sciences, 79(3):143.
2. Castle, R. D., Williams, M. A., Bushell, W. C., Rindfleisch, J. A. et al. (2021). Implications for Systemic Approaches to COVID-19: Effect Sizes of Remdesivir, Tocilizumab, Melatonin, Vitamin D3, and Meditation. Journal of Inflammation Research, 14, 4859–4876.
3. Camp, O. G., Bai, D., Gonullu, D. C., Nayak, N., & Abu-Soud, H. M. (2021). Melatonin Interferes with COVID-19 at Several Distinct ROS-related Steps. Journal of Inorganic Biochemistry, 223, 111546.
4. Ryback, R., & Eirin, A. (2022). Mitochondria, a Missing Link in COVID-19 Heart Failure and Arrest?. Frontiers in Cardiovascular Medicine, 8, 830024.
5. Su, W. L., Wu, C. C., Wu, S. V., Lee, M. C., Liao, M. T., Lu, K. C., & Lu, C. L. (2022). A Review of the Potential Effects of Melatonin in Compromised Mitochondrial Redox Activities in Elderly Patients With COVID-19. Frontiers in Nutrition, 9, 865321.
6. Lee, R. U., & Glickman, G. L. (2021). Sleep, Circadian Health and Melatonin for Mitigating COVID-19 and Optimizing Vaccine Efficacy. Frontiers in Neuroscience, 15, 711605.
7. Brusco, L., Cruz, P., Cangas, A., Rojas, C., Vigo, D. & Cardinali, D. (2021). Efficacy of Melatonin in Non-Intensive Care Unit Patients with COVID-19 Pneumonia and Sleep Dysregulation. Melatonin Research. 4, 1 (Jan. 2021), 173-188.
8. Bologna, C., Madonna, P., & Pone, E. (2021). Efficacy of Prolonged-Release Melatonin 2 mg (PRM 2 mg) Prescribed for Insomnia in Hospitalized Patients for COVID-19: A Retrospective Observational Study. Journal of Clinical Medicine, 10(24), 5857.
9. Lan, S. H., Lee, H. Z., Chao, C. M., Chang, S. P., Lu, L. C., Lai, C. C. (2022). Efficacy of Melatonin in the Treatment of Patients with COVID-19: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Journal of Medical Virology, 94: 2102- 2107.
10. DiNicolantonio, J. J., McCarty, M. & Barroso-Aranda, J. (2021). Melatonin May Decrease Risk for and Aid Treatment of COVID-19 and Other RNA Viral Infections. Open Heart, 8:e001568.
11. Brown, G. M., Pandi-Perumal, S. R., Pupko, H., Kennedy, J. L., & Cardinali, D. P. (2021). Melatonin as an Add-On Treatment of COVID-19 Infection: Current Status. Diseases (Basel, Switzerland), 9(3), 64.
12. Fogleman, C., Cohen, D., Mercier, A., Farrell, D., et al. (2022). A Pilot of a Randomized Control Trial of Melatonin and Vitamin C for Mild-to-Moderate COVID-19. The Journal of the American Board of Family Medicine, 35 (4) 695-707.
13. Sánchez-Rico, M., de la Muela, P., Herrera-Morueco, J. J., Geoffroy, P. A. et al. (2022). Melatonin Does Not Reduce Mortality in Adult Hospitalized Patients with COVID-19: A Multicenter Retrospective Observational Study. Journal of Travel Medicine, 29(3), taab195.
14. Sahu, N., Ramzy, J., Corwin, D., Rahman, A. et al. (2021). Retrospective Review of Melatonin in Patients with COVID-19. Chest Journal, 160 (4), Supplement A560.
15. Reiter, R. J., Abreu-Gonzalez, P., Marik, P. E., Dominguez-Rodriguez, A. (2020). Therapeutic Algorithm for Use of Melatonin in Patients With COVID-19. Frontiers in Medicine, 7.
16. Giménez, V. M., Inserra, F., Tajer, C. D., Mariani, J. et al. (2020). Lungs as Target of COVID-19 Infection: Protective Common Molecular Mechanisms of Vitamin D and Melatonin as a New Potential Synergistic Treatment. Life Sciences, 254.
17. Lavialle, M., Champeil-Potokar, G. et al. (2008). An (n-3) Polyunsaturated Fatty Acid-Deficient Diet Disturbs Daily Locomotor Activity, Melatonin Rhythm, and Striatal Dopamine in Syrian Hamsters. Journal of Nutrition, 138(9), 1719-24.
Popular posts


Related posts