Vitamin D and COVID-19: Up to the Minute
Vitamin D has made headlines many times these last few years of the pandemic.
The excitement surrounding vitamin D makes sense. Studies show that having healthy vitamin D levels seems to protect against severe COVID-19 infection and death. And many scientists have argued that this affordable “sunshine vitamin” could be key to saving lives.
But how exactly does vitamin D impact our immune system if we get an infection? And how much vitamin D do we need? We look closer in this Part II of our series on the nutrients that affect immune health.
Why Vitamin D May Help Fight COVID-19
Vitamin D is best known for its bone benefits. But people have recognized vitamin D’s positive impact on the immune system for some time. Before the discovery of penicillin, doctors often treated tuberculosis patients with two potent vitamin D sources: cod liver oil and sunbathing [1].
Today, we know that vitamin D not only helps fight bacterial infections like tuberculosis, but that it has anti-fungal and antiviral properties, too [2]. Let’s highlight a few ways that vitamin D protects immune health – especially in the context of COVID-19.
Shields Against Complications
When a person gets COVID-19, the virus often disturbs the Renin-Angiotensin-Aldosterone System (or RAAS, for short). The RAAS regulates our blood pressure and blood volume, among other things.
COVID-19 disrupts the RAAS by sneaking into the cell through the ACE2 receptor. As a key enzyme of the RAAS, ACE2 influences whether our blood vessels contract or dilate. When the virus binds to the ACE2 receptor, it can cause a host of problems, like high blood pressure, inflammation, and oxidative stress [3].
Vitamin D regulates the RAAS. If vitamin D levels are low, the RAAS becomes overactive. Having a hyperactive RAAS sets the stage for a “perfect storm” when COVID-19 hits [4]. It makes it more likely that the person will experience serious complications, like acute respiratory distress syndrome and organ failure [4, 5].
The good news is that when vitamin D levels normalize, the vitamin can check an overactive RAAS [4, 5]. By inhibiting RAAS overstimulation, vitamin D may significantly improve COVID-19 outcomes.
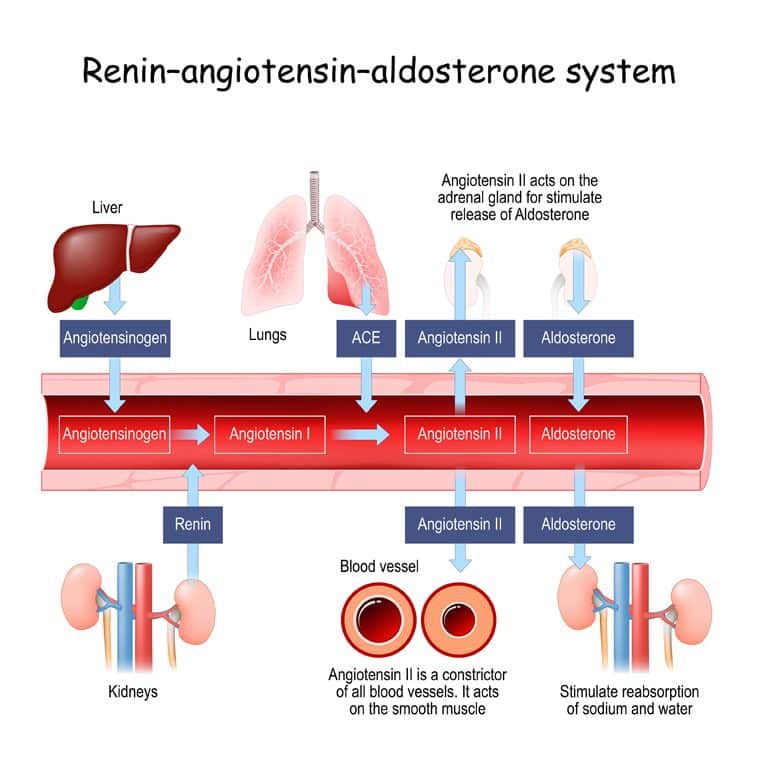
RAAS regulator: Healthy vitamin D levels keep the Renin-Angiotensin-Aldosterone System in check.
Supports the Mitochondria
SARS-CoV-2 – the virus behind COVID-19 – replicates by targeting protein-making machinery in the mitochondria. This has serious consequences since the mitochondria are the power generators of the cell and communication hub for the immune response.
Vitamin D can step in as an antioxidant to stabilize the mitochondria’s membrane potential. This antioxidant function curtails SARS-CoV-2’s ability to induce cell damage.
Unfortunately, if a person has low vitamin D levels, the lack of antioxidant protection makes it more likely they will experience mitochondrial dysfunction and cell death [4].
Stimulates Antimicrobial Peptides
Vitamin D stimulates the production of antimicrobial peptides called cathelicidin and defensins.
Working almost like antibiotics, cathelicidin and defensins inhibit the growth of harmful bacteria and viruses [5, 6]. They also play a crucial role in both innate and adaptive immunity.
Currently, researchers are examining how these peptides affect SARS-CoV-2 specifically. Some studies indicate that these peptides may inhibit some of the virus’ enzymatic activity [7] and block viral entry into the cell [8]. However, more research is still needed.
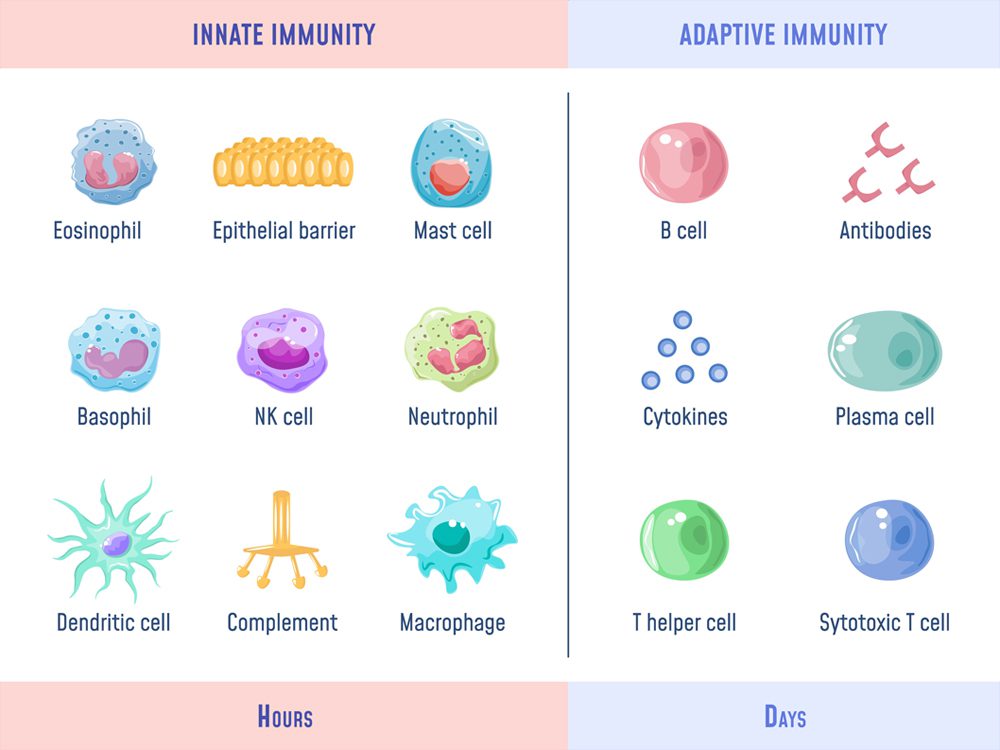
The body’s defense system: Vitamin D plays a role in both the innate and adaptive immunity. Innate immunity depends on your inborn genetic makeup, while adaptive immunity depends on defenses that develop when you’re exposed to different pathogens.
Reduces the Risk of a Cytokine Storm
Vitamin D also inhibits the protein complex called NF-kB. NF-kB plays a big role in inflammation. NF-kB activation triggers the production of pro-inflammatory cytokines, chemokines, and T cells.
Excessive NF-kB activation can set the stage for the dangerous cytokine storm, which is associated with greater COVID-19 severity [9]. By inhibiting NF-kB, vitamin D may well be a helpful tool for preventing some of COVID-19’s more deadly consequences.
Provides Cardiovascular Benefits
COVID-19 can have devastating effects on the heart. As one example, the CDC reported that COVID-19 patients had nearly 16 times the risk for myocarditis compared to patients who did not have COVID-19 [10].
Vitamin D’s cardiovascular benefits can offer many advantages. Notably, vitamin D prevents the death of endothelial cells [4]. Endothelial cells line the inside of the heart and blood vessels. They provide substances that control the heart’s pumping action, as well as enzymes that control blood clotting, immune function, and platelet adhesion.
All the ways vitamin D protects the heart are still being untangled. However, we know that when a person gets enough vitamin D, it can reduce vascular calcification and atherosclerosis, as well as support healthy heart tissue [11].
Better outcomes: In trials, researchers have found that higher levels of vitamin D are linked with lower risk of severe disease and death.
How Has Vitamin D Performed in COVID-19 Trials?
Studies show there is a significant association between vitamin D deficiency and the risk of having a severe case of COVID-19. The good news is that when vitamin D levels normalize, it may improve COVID-19 outcomes.
A big question is whether treating COVID-19 patients with vitamin D supplements can also have beneficial effects. Here, the evidence looks promising so far:
• One study from Spain found that COVID-19 patients who received vitamin D3 supplements had a lower risk of infection, severe disease and mortality compared to unsupplemented patients [12].
• A study from England also found that vitamin D supplementation seemed to protect against death, regardless of the person’s initial vitamin D levels [13].
• Other studies have similarly found that vitamin D supplementation may benefit mildly symptomatic patients [3], result in shorter treatment times, and reduce mortality rates [11].
Still, the results are not conclusive, and questions remain. For instance, in one study from India, a single dose of 60,000 IUs of vitamin D did not make any difference for COVID-19 outcomes [14].
The variable results have led some scientists to wonder if the timing and duration of the intervention matters. One study from France seemed to suggest this. It found that patients who received regular doses of 50,000 IUs before getting sick had better outcomes than patients who received 80,000 IUs a few hours after being diagnosed with COVID-19 [15].
Vitamin D + Vaccination
Access to vaccinations has changed the COVID-19 landscape —and there is evidence that vitamin D can offer benefits for the vaccinated as well [16].
The authors of one German study strongly recommended combining vaccination with vitamin D supplementation to strengthen the immune system of the entire population.
According to the researchers, this intervention would save lives, increase the success of vaccination, and potentially lower the need for future lockdowns. In addition, it could save billions of dollars, “as vitamin D is inexpensive and—together with vaccines — provides an excellent opportunity to get COVID-19 under control” [16].
The Benefits of Omega-3 + Vitamin D
Vitamin D is even more effective when accompanied by omega-3 fatty acids.
As discussed in Part I, omega-3s have their own benefits for COVID-19 patients. Similarly to vitamin D, omega-3s reduce inflammation and oxidative stress, but through complementary mechanisms. That’s why the combination may better support your body’s ability to fight cell damage caused by the virus.
Furthermore, research suggests that omega-3s may potentiate circulating vitamin D levels. In one study, patients who took omega-3 supplements for 3 months had higher vitamin D levels compared to baseline, even without additional vitamin D [17].
Lastly, studies from other health areas have highlighted the benefits of taking vitamin D together with omega-3s [18, 19]. Given the precedent, it’s plausible those advantages would extend to COVID-19 patients as well.

Daily vitamin D source: Omega Cure Extra Strength provides 1400 IUs of vitamin D3 per serving, plus 3000 mg of EPA/DHA omega-3s.
Vitamin D Dose Questions
Despite vitamin D’s many benefits, most Americans pay little attention to their daily vitamin D intake. They might think that they are getting enough vitamin D from their multivitamin or their daily glass of milk.
How Many People Are Vitamin D Deficient?
Unfortunately, an estimated 42% of Americans have low vitamin D levels. Those rates are higher in people who are older, obese, or have high blood pressure. Vitamin D deficiency is also more common among Hispanic and Black people.
Because the best source of vitamin D is the sun, vitamin D deficiencies can also result from long-term indoor activities. Living in cities that are cloudy or with tall buildings that block out the sunshine doesn’t help, either.
In addition, there’s a seasonality aspect as well. In most cities located above 35° North latitude, people do not synthesize adequate amounts of vitamin D from November through February [20]. No wonder a robust body of research shows the need to monitor our vitamin D levels!
How Much Vitamin D Do You Need for Good Immune Health?
The Recommended Dietary Allowance is currently 600 IUs of vitamin D each day. That level goes up to 800 IUs a day for those who are older than age 70. With that said, vitamin D researchers have cited far higher intake levels of 4000 – 10,000 IUs for people at risk for COVID-19 [5, 16].
Since dose depends on many individual factors, it can often be more reliable to measure the circulating vitamin D levels in your body. Levels between 40 to 60 ng/mL are considered optimal [3, 5].
While eating a healthy diet is wise, few foods are naturally rich in vitamin D. One needs to couple sun exposure with fortified foods to get enough. If that’s challenging, supplements can help you hit your target.
There are limits, to be sure. Taking massive amounts of vitamin D can work against you, so be mindful of the correct dosage in your instance.
Getting Enough Vitamin D Every Day
There’s a lot of things to keep in mind with vitamin D. It’s a workhorse of wonder when the body has an adequate supply. But if we get less vitamin D than we need, it opens the gates to many health problems.
Since vitamin D deficiency is all too common in the United States, most of us need to be mindful of our daily intake. That can take the form of regularly spending time outside in the sun, eating more vitamin D-rich foods, and taking a daily dose of cod liver oil.
For those looking to increase their intake of both omega-3s and vitamin D, we have an easy solution. Each vial of Omega Cure Extra Strength and Omega Restore contains 1400 IUs of vitamin D3, for an extra boost of good health.
For More Restful Sleep and Energy
Experience the Omega3 Innovations difference for yourself with the most effective fish oil supplement on the market.
Buy Now
References:
1. Aranow, C. (2011). Vitamin D and the Immune System. Journal of Investigative Medicine: The Official Publication of the American Federation for Clinical Research, 59(6), 881–886.
2. White, J. H. (2022). Emerging Roles of Vitamin D-Induced Antimicrobial Peptides in Antiviral Innate Immunity. Nutrients, 14(2), 284.
3. Bae, J. H., Choe, H. J., Holick, M. F., & Lim, S. (2022). Association of Vitamin D Status with COVID-19 and Its Severity : Vitamin D and COVID-19: A Narrative Review. Reviews in Endocrine & Metabolic Disorders, 1–21.
4. de Las Heras, N., Martín Giménez, V. M., Ferder, L., Manucha, W., & Lahera, V. (2020). Implications of Oxidative Stress and Potential Role of Mitochondrial Dysfunction in COVID-19: Therapeutic Effects of Vitamin D. Antioxidants (Basel, Switzerland), 9(9), 897.
5. Peng, M. Y., Liu, W. C., Zheng, J. Q., et al. (2021). Immunological Aspects of SARS-CoV-2 Infection and the Putative Beneficial Role of Vitamin-D. International Journal of Molecular Sciences, 22(10), 5251.
6. Chung, C., Silwal, P., Kim, I., Modlin, R. L., & Jo, E. K. (2020). Vitamin D-Cathelicidin Axis: At the Crossroads between Protective Immunity and Pathological Inflammation during Infection. Immune Network, 20(2), e12.
7. Zhang, R., Jiang, X., Qiao, J., Wang, Z., Tong, A., Yang, J., Yang, S., & Yang, L. (2021). Antimicrobial Peptide DP7 with Potential Activity Against SARS Coronavirus Infections. Signal Transduction and Targeted Therapy, 6(1), 140.
8. Ghosh, S. K. & Weinberg, A. (2021). Ramping Up Antimicrobial Peptides Against Severe Acute Respiratory Syndrome Coronavirus-2. Frontiers in Molecular Biosciences, 8.
9. Davies, D. A., Adlimoghaddam, A., & Albensi, B. C. (2021). The Effect of COVID-19 on NF-κB and Neurological Manifestations of Disease. Molecular Neurobiology, 58(8), 4178–4187.
10. Boehmer, T. K, Kompaniyets, L., Lavery, A. M., Hsu, J. et al. (2021). Association Between COVID-19 and Myocarditis Using Hospital-Based Administrative Data — United States, March 2020–January 2021. Centers for Disease Control and Prevention.
11. Purnama, D. I., Kusuma, W. L., Purnama, D. K., et al. (2021). The Role of Vitamin D and Cardiovascular Risk in COVID-19 Patients. Cardiovascular and Metabolic Science, 32(3):149-156.
12. Oristrell, J., Oliva, J. C., Casado, E., Subirana, I., Domínguez, D., Toloba, A., Balado, A., & Grau, M. (2022). Vitamin D Supplementation and COVID-19 Risk: A Population-Based, Cohort Study. Journal of Endocrinological Investigation, 45(1), 167–179.
13. Ling, S. F., Broad, E., Murphy, R., Pappachan, J. M., Pardesi-Newton, S., Kong, M. F., & Jude, E. B. (2020). High-Dose Cholecalciferol Booster Therapy is Associated with a Reduced Risk of Mortality in Patients with COVID-19: A Cross-Sectional Multi-Centre Observational Study. Nutrients, 12(12), 3799.
14. Jevalikar, G., Mithal, A., Singh, A., Sharma, R., Farooqui, K. J., Mahendru, S., Dewan, A. & Budhiraja, S. (2021). Lack of Association of Baseline 25‑Hydroxyvitamin D Levels with Disease Severity and Mortality in Indian Patients Hospitalized for COVID‑19. Nature, Scientifc Reports, 11:625.
15. Annweiler, G., Corvaisier, M., Gautier, J., Dubée, V., Legrand, E., Sacco, G., Annweiler, C. (2020). Vitamin D Supplementation Associated to Better Survival in Hospitalized Frail Elderly COVID-19 Patients: The GERIA-COVID Quasi-Experimental Study. Nutrients, 2(11):3377.
16. Borsche, L., Glauner, B., & von Mendel, J. (2021). COVID-19 Mortality Risk Correlates Inversely with Vitamin D3 Status, and a Mortality Rate Close to Zero Could Theoretically Be Achieved at 50 ng/mL 25(OH)D3: Results of a Systematic Review and Meta-Analysis. Nutrients, 13(10):3596.
17. Razavi M, Jamilian M, Samimi M, Afshar Ebrahimi F, Taghizadeh M, et al. (2017). The Effects of Vitamin D and Omega-3 Fatty Acids Co-Supplementation on Biomarkers of Inflammation, Oxidative Stress and Pregnancy Outcomes in Patients with Gestational Diabetes. Nutrition & Metabolism (London), 14:80.
18. Scrimgeour, A. G., Condlin, M. L., Loban, A., & DeMar, J. C. (2021). Fatty Acids and Vitamin D Decrease Plasma T-Tau, GFAP, and UCH-L1 in Experimental Traumatic Brain Injury. Frontiers in Nutrition, 8.
19. Tay, C. (2019). Combined Vitamin D3 and Omega-3 Supplementation May Have Bone, Heart, and Kidney Benefits. NutraIngredients.
20. Cesari, M., Incalzi, R. A., Zamboni, V., & Pahor, M. (2011). Vitamin D Hormone: A Multitude of Actions Potentially Influencing the Physical Function Decline in Older Persons. Geriatrics & Gerontology International, 11(2), 133–142.
Popular posts


Related posts