Why Vitamin D Deficiency Is More Serious Than You Think
I admit it. It’s hard for me to see my husband stretched out in the backyard on a lounge chair in his altogether, taking a 20-minute sunbath, when I thought he said he was going to clean out the garage.
I really can’t complain though. After all, he’s loading up on the wonderful sunshine vitamin – Vitamin D. As research indicates, he might actually be strengthening his bones and muscles, decreasing his odds of getting certain cancers and Alzheimer’s disease, and helping his cardiovascular system.
What I really should do is stop grumbling under my breath, and join him.
Where Do You Get Vitamin D?
While it’s called a “vitamin”, vitamin D is technically classified as a hormone (like melatonin). Chemically, it is a steroid, or secosteroid to be exact.
While we receive small amounts of vitamin D from some foods (e.g. certain types of fish, eggs, and fortified dairy products), the primary way we synthesize vitamin D is through sun exposure. When sunlight hits the skin, it starts a series of chemical reactions that ultimately create vitamin D within the body.
Unfortunately, there are many hurdles that keep us out of the sunshine, from living in cities with tall buildings that block the sun to using synthetic sunscreens, to staying indoors all day. Even the latitude of your hometown can make a big difference in terms of your vitamin D status throughout the year. For instance, if you live above 35° North latitude (in cities like New York, Chicago and Seattle), you likely get little to no vitamin D from the sun from November to February (1)!

Besides certain types of fish and some omega-3 oils, relatively few foods contain significant amounts of vitamin D. Fortified dairy products, eggs, and some types of mushrooms can also provide small amounts.
Why Is Vitamin D Important?
Much of the original interest in vitamin D centered on its bone benefits. Scientists discovered vitamin D in the 1920s while they were investigating why cod liver oil (a traditionally good source of vitamin D) seemed to prevent the development of rickets and bone disease in children (2). The scientists soon determined that the lack of vitamin D led to bone malformations, especially in the arms and legs.
While vitamin D’s bone benefits are certainly important, most of the research in the last 15 years has concentrated on its immune advantages. Today, it’s understood that vitamin D receptors are found in many parts of the body totally unrelated to bone metabolism – including the brain, heart, intestines, colon, prostate, breasts, and immune cells (3, 4). We also know that vitamin D is important for turning on and off genes inside those cells (5).
How Vitamin D Supports the Immune System
Vitamin D serves a variety of functions in our immune system. For one, vitamin D acts like a messenger through the circulatory system, helping with cell signaling. You’ll often see researchers describe vitamin D’s autocrine and paracrine signaling abilities. “Autocrine” refers to the individual cells talking to themselves, while “paracrine” refers to cells communicating with other cells nearby (sort of like two students passing notes to each other in class).
In the initial phase of an infection, our skin, tears, and mucus try to set up a physical barrier against incoming viruses and bacteria. When that doesn’t work, vitamin D nudges our Toll-like receptors to sound the alarm to our immune cells (6). It is these receptors which both recognize the “fingerprints” (or patterns) in pathogens and initiate a process to eliminate them.

During an infection, cells have to communicate with each other to effectively mount a local infection response. Vitamin D facilitates their signaling.
Vitamin D’s role doesn’t end there. Here is a simplified explanation of some of the other ways vitamin D reduces the risk of infections, courtesy of William Grant, PhD et al (7):
1. Maintains Junctions
Vitamin D maintains tight junctions, adherens junctions, and gap junctions between cells. This is important since viruses do their best to break through these junctions in order to further spread into the body. The more solid these junctions are, the more adept your body is at preventing entry in the first place.
2. Induces Antimicrobial Peptides
Antimicrobial peptides called cathelicidins and defensins help damage invading pathogens. Interestingly, these peptides may have advantages over traditional antibiotics due to their anti-bacterial, anti-fungal, anti-virus, and anti-cancer effects – and may even overcome bacterial drug-resistance (8). In short, they’re incredible at fighting infections.
3. Strengthens Cellular Immunity
Getting enough vitamin D suppresses the overproduction of pro-inflammatory cytokines. It also increases the expression of anti-inflammatory cytokines (which can be beneficial for recovery).
4. Modulates Immune Cells
As mentioned above, vitamin D receptors are found in nearly all of the immune cells and impacts them accordingly. To name just a few of its effects, vitamin D modulates the expression and types of T cells in the body. It also increases the B cells’ apoptotic effect on infected cells, and recruits neutrophils, monocyte-macrophages, and dendritic cells to the infection site (9). Thanks to these varied benefits, the body is more easily able to destroy infected cells, clean them out of the system, and start the recovery process.
Our Immune Cells
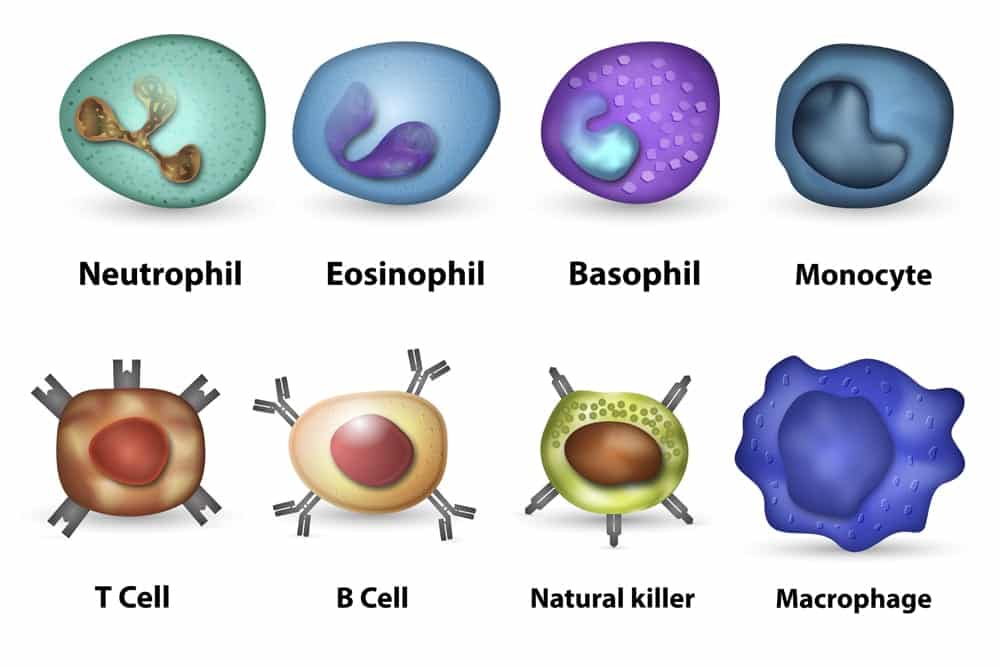
Vitamin D modulates our immune cells in a variety of ways, helping our bodies eliminate pathogens and facilitate recovery.
How Vitamin D Helps Fight Infectious Diseases
In a world where antibiotics are losing their effect and the risk of infectious diseases is on the rise, it’s important to find greater ways to naturally boost our bodies’ defenses. New understandings about the biological channels associated with vitamin D could point the way to much-needed, cost-effective health treatments.
Vitamin D and COVID-19
Most recently, scientists are trying to clarify the relationship between vitamin D and COVID-19. A study in May showed a strong correlation between low vitamin D levels and a doubling of complications and mortality rates from COVID-19 (11).
Of note, the arrival of COVID-19 coincided with the end of winter, when vitamin D levels were already at an all time low for a large portion of the globe (7). While vitamin D deficiency is likely not the only factor responsible for increased complications, it certainly could be a contributing variable and has spurred increased interest in understanding vitamin D’s immunological mechanisms.
Vitamin D Questions
In spite of its promise, there is still much to learn about the effects of vitamin D. For instance, while we know that vitamin D deficiency has been consistently linked with an increased risk of respiratory infections, vitamin D supplementation hasn’t performed consistently in clinical trials.
Scientists speculate that in order for vitamin D supplementation to work, more research needs to be done on optimal dosage, frequency, timing of intervention, and combinations with other treatments(10). In that sense, the questions surrounding vitamin D supplementation are not so different from the ones being asked about fish oil.
What Are the Effects of Vitamin D Deficiency?
Vitamin D deficiency (also known as hypovitaminosis D) is strongly correlated with the increased incidence and severity of numerous age-related diseases. These can include – but are not limited to – obesity, insulin resistance, type 2 diabetes, hypertension, pregnancy complications, memory disorders, osteoporosis, autoimmune diseases, certain cancers, and system inflammatory diseases (12).
How Prevalent Is Vitamin D Deficiency?
How many people are at risk of vitamin D deficiency depends on how the deficiency is defined (<20 vs. <30 ng/mL) (13).
Nevertheless, it’s estimated that at least 40% of adult Americans have insufficient vitamin D levels (14, 10), although certain populations are more vulnerable than others. People have an increased risk if they: are older than 50, have darker skin pigmentation, receive limited light exposure during the day, are pregnant, or are overweight (15).
Women are more likely to be vitamin D deficient than men (15). In addition, we also know that certain types of drugs can reduce vitamin D concentrations (including antibiotics, NSAIDs, and antihypertensives) (7).

As we age, our skin synthesizes vitamin D less effectively. This one of the reasons why individuals older than 50 (and especially those older than 65) are at a higher risk for vitamin D deficiency.
Can I Get Too Much Vitamin D?
Whether you talk to bone health or immunity experts, there are conflicting beliefs about what’s considered too little vitamin D. For instance, the Endocrine Society defines blood levels lower than 30 ng/mL as insufficient, whereas the Institute of Medicine defines insufficiency as lower than 20 ng/ml (10).
There is agreement, however, that you should not have blood levels higher than 150 ng/ml. Fortunately, getting up to those elevated blood levels is exceedingly rare. It is impossible to get excessive amounts of vitamin D from either sunlight or diet. Additionally, you would have to take high doses of vitamin D supplements over several months in order to obtain toxic levels of vitamin D (15, 1).
Note: During periods of elevated infection risk, getting high enough levels should be a priority. For an adult, that would mean blood levels between 40-60 ng/ml (16).
The Right Amount of Vitamin D
Again, the recommended daily intake of vitamin D depends on who you ask. However, after correcting for a vitamin D deficiency, most people should be able to maintain healthy vitamin D levels with a daily intake of between 1000-4000 IU (25-100 mcg).
While getting vitamin D from the sun is probably the most efficient and cost-effective source of vitamin D, intense sun exposure can cause wrinkles and skin cancer. On the other hand, a sufficient vitamin D status can help protect against several types of cancers, melanoma, and other diseases (12).
In order to reconcile the sun’s healthful and harmful effects, most experts agree that the key is practicing healthy sun exposure and avoiding sunburn. You don’t need to bask in the sun for hours to get sufficient vitamin D levels! For people with light skin pigmentation, for example, it’s been estimated that getting as little as 5 – 10 minutes of sun exposure on one’s arms and legs in the middle of a summer day can provide up to 3000 IUs of vitamin D (1).

In addition to the omega-3s, Omega Cure Extra Strength and Omega Restore contain 1400 IUs of added vitamin D3 per daily serving.
How Much Vitamin D Is in My Omega-3 Supplement?
Omega-3s and vitamin D have a long history together. As mentioned above, vitamin D was first synthesized from cod liver oil. Furthermore, certain types of omega-3-rich fish (including salmon, sardines and herring) remain some of the best vitamin D food sources.
While cod liver oil was historically considered a good source of vitamin D, the amount of natural vitamin D in cod liver oil today will entirely depend on how that brand is purified. Purifying any omega-3 oil is essential in order to remove harmful pollutants, like mercury and PCBs. However, careful purification also means that most naturally-occuring vitamins are significantly reduced or removed in the process too.
Why Our Omega-3 Fish Oil Is Different
Omega Cure® is a full-spectrum cod liver oil, meaning it retains a broader range of fatty acids and nutrient cofactors than other omega-3 oils.
Because of the careful way we purify our Omega Cure oil, however, almost all of the natural vitamin D in the oil is lost. For those wanting to increase their vitamin D levels, we add back 1400 IUs of vitamin D into our Omega Cure Extra Strength and Omega Restore vials – the same level historically found in cod liver oil.
We believe that omega-3s and vitamin D are excellent partners and ultimately belong together. Both are fat soluble, crucial for cell membrane function, and help to reduce inflammation levels. Furthermore, omega-3s may be important for vitamin D activation and metabolism (17).
The Future of Vitamin D Research
Vitamin D regulates so many important physiological functions that we’ve only scratched the tip of the iceberg in this article. And we still have much to learn about this fascinating hormone. Questions like, “What’s the optimal vitamin D intake for various conditions,” and “What is the safest and most effective way to get enough vitamin D” are all hotly contested topics. Hopefully in the coming years, research will provide us with more answers.
In the meantime, I’m paying closer attention to my vitamin D levels and re-evaluating my relationship with the sun. Now, when I see my husband basking his body outside, I put away my to-do list for a while.
Because getting enough vitamin D is a daily task that I want to check off with confidence.
An Effective Omega-3 Dose, Made Simple
Experience the Omega3 Innovations difference for yourself with the most effective fish oil supplement on the market.
Buy Now
References:
1. Cesari, M., Incalzi, R. A., Zamboni, V., & Pahor, M. (2011). Vitamin D Hormone: A Multitude of Actions Potentially Influencing the Physical Function Decline in Older Persons. Geriatrics & Gerontology International, 11(2), 133–142.
2. Wilton P. (1995). Cod-Liver Oil, Vitamin D and the Fight Against Rickets. CMAJ : Canadian Medical Association Journal = Journal de l’Association Medicale Canadienne, 152(9), 1516–1517.
3. Aranow C. (2011). Vitamin D and the Immune System. Journal of Investigative Medicine: The Official Publication of the American Federation for Clinical Research, 59(6), 881–886.
4. Marino, R., & Misra, M. (2019). Extra-Skeletal Effects of Vitamin D. Nutrients, 11(7), 1460.
5. Wacker, M., & Holick, M. F. (2013). Vitamin D – Effects on Skeletal and Extraskeletal Health and the Need for Supplementation. Nutrients, 5(1), 111–148.
6. Arababadi, K. M., Nosratabadi, R., Asadikaram, G. (2018). Vitamin D and Toll Like Receptors. Life Sciences, 203, 105-111.
7. Grant, W. B., Lahore, H., McDonnell, S. L., Baggerly, C. A., French, C. B., Aliano, J. L., & Bhattoa, H. P. (2020). Evidence that Vitamin D Supplementation Could Reduce Risk of Influenza and COVID-19 Infections and Deaths. Nutrients, 12(4), 988.
8. van Harten, R. M., van Woudenbergh, E., van Dijk, A., & Haagsman, H. P. (2018). Cathelicidins: Immunomodulatory Antimicrobials. Vaccines, 6(3), 63.
9. Panfili, F. M., Roversi, M., D’Argenio, P., Rossi, P., Cappa, M., & Fintini, D. (2020). Possible Role of Vitamin D in Covid-19 Infection in Pediatric Population. Journal of Endocrinological Investigation, 1–9.
10. Martens, P. J., Gysemans, C., Verstuyf, A., & Mathieu, A. C. (2020). Vitamin D’s Effect on Immune Function. Nutrients, 12(5), 1248.
11. Northwestern University. (2020, May 7). Vitamin D Levels Appear to Play Role in COVID-19 Mortality Rates: Patients with Severe Deficiency Are Twice as Likely to Experience Major Complications. ScienceDaily.
12. Wimalawansa S. J. (2019). Vitamin D Deficiency: Effects on Oxidative Stress, Epigenetics, Gene Regulation, and Aging. Biology, 8(2), 30.
13. Cesareo, R. et al. (2018). Italian Association of Clinical Endocrinologists (AME) and Italian Chapter of the American Association of Clinical Endocrinologists (AACE) Position Statement: Clinical Management of Vitamin D Deficiency in Adults. Nutrients, 10(5), 546.
14. Sowah, D., Fan, X., Dennett, L., Hagtvedt, R., & Straube, S. (2017). Vitamin D Levels and Deficiency with Different Occupations: A Systematic Review. BMC Public Health, 17(1), 519.
15. Meehan, M., & Penckofer, S. (2014). The Role of Vitamin D in the Aging Adult. Journal of Aging and Gerontology, 2(2), 60–71.
16. Martín Giménez, V. M., Inserra, F., Tajer, C. D., Mariani, J., Ferder, L., Reiter, R. J., & Manucha, W. (2020). Lungs as Target of COVID-19 Infection: Protective Common Molecular Mechanisms of Vitamin D and Melatonin as a New Potential Synergistic Treatment. Life Sciences, 254, 117808.
17. Lee, S. M., Lee, M. H., Son, Y. K., Kim, S. E., & An, W. S. (2019). Combined Treatment with Omega-3 Fatty Acid and Cholecalciferol Increases 1,25-Dihydroxyvitamin D Levels by Modulating Dysregulation of Vitamin D Metabolism in 5/6 Nephrectomy Rats. Nutrients, 11(12), 2903.
Popular posts


Related posts