Interleukin-6: The Inflammation Marker You Need to Know
By now, most people have learned that surviving COVID-19 often comes down to having a well-performing immune system and low levels of chronic inflammation. But how do you know if your immune system is in good shape?
Promising new research shows that interleukin levels might be one of the strongest predictors of future health outcomes, including for COVID-19 patients. Unfortunately, the general public (and many health care professionals) aren’t aware of the importance of dysregulated interleukins.
This article aims to lay out a simplified explanation of what interleukin-6 does – and what factors can help reduce high levels of interleukin-6 in the body.
Do I Have a Dysfunctional Immune System?
There are three ways to get an indication of having a higher-than-average immune risk:
1. If you are older and have underlying health issues (e.g. diabetes, high blood pressure, severe arthritis, cancer, dementia), or your immune system is compromised by stress, poor sleep, or malnourishment.
2. If you frequently use antibiotics, cortisone, or are undergoing cancer treatment.
3. If your blood samples show increased sedimentation rates, abnormal blood cells, or dysregulated interleukins.
These factors are especially good to be aware of since – in today’s COVID-19 era – some epidemiologists think that one of the best public health strategies may be to identify people at increased risk of infection complications and shelter them from bacterial or viral exposure (1).
What Are Interleukins?
Interleukins are cell proteins that are heavily involved in controlling our immune system and ensuring that it’s responsive to invading microbes. Having too many – or too few – of these interleukins is equally bad and puts us at risk. These immune system markers can be measured (typically through blood or saliva tests) in order to get a better indication of our bodies’ readiness to respond to infections and diseases.
While there are many different interleukins, let’s focus on interleukin-6 (IL-6), which has been heavily researched since its discovery over 30 years ago.

Health problems arise when your interleukin-6 levels are chronically out of balance. In most cases, this means an overproduction of IL-6.
What Does Interleukin-6 Do?
IL-6 has been described as a sort of “Dr. Jekyll and Mr. Hyde” molecule, with both pro-inflammatory and anti-inflammatory functions (2).
Because of its dual role in the body, some conditions – like immunodeficiency – are characterized by too low levels of IL-6 (3). In the majority of cases, however, people suffer from having too high levels.
High IL-6 is strongly associated with chronic inflammation and most pro-inflammatory diseases, including obesity, arthritis, cancers, and much more. For this reason, IL-6 is typically used as an inflammation marker in research studies (4). While IL-6 will not give you a specific diagnosis of what’s wrong, you can think of it as an alarm bell.
A Predictor of Early Death
High IL-6 levels are also a strong predictor of all-cause early mortality in older adults (2, 4). Particularly, if a patient’s IL-6 levels do not go down during treatment for cancer or severe infections, it is an ominous sign as to the patient’s outcome (2).
This pattern holds true for COVID-19 patients as well. Patients who were classified as “critically ill” with COVID-19 had higher IL-6 levels at the start of their illness, and their levels continued to rise (rather than decrease) despite treatment (5).
How IL-6 Influences the Microbiome
IL-6 is involved in many aspects of our immune system, including modulating the balance of our gut bacteria. When levels are high, it indicates that the integrity of the intestinal wall may be in jeopardy. That’s because IL- 6 increases intestinal leakage (also known as ‘leaky gut’), which allows bad bacteria or viruses to enter our bodies (6, 7).
Microbiome health also has a profound effect on IL-6: “Bad” endotoxin-producing bacteria stimulate Il-6 production (8).
As we have written about before, microbiome imbalances may be the main driver of chronic inflammation and a dysregulated immune system. Since IL-6 has a strong influence on the microbiome, it’s not strange that IL-6 is a crucial player in health and disease.
Even if you have chronic inflammation issues and high levels of interleukin-6, there are numerous evidence-based ways to bring those levels down.
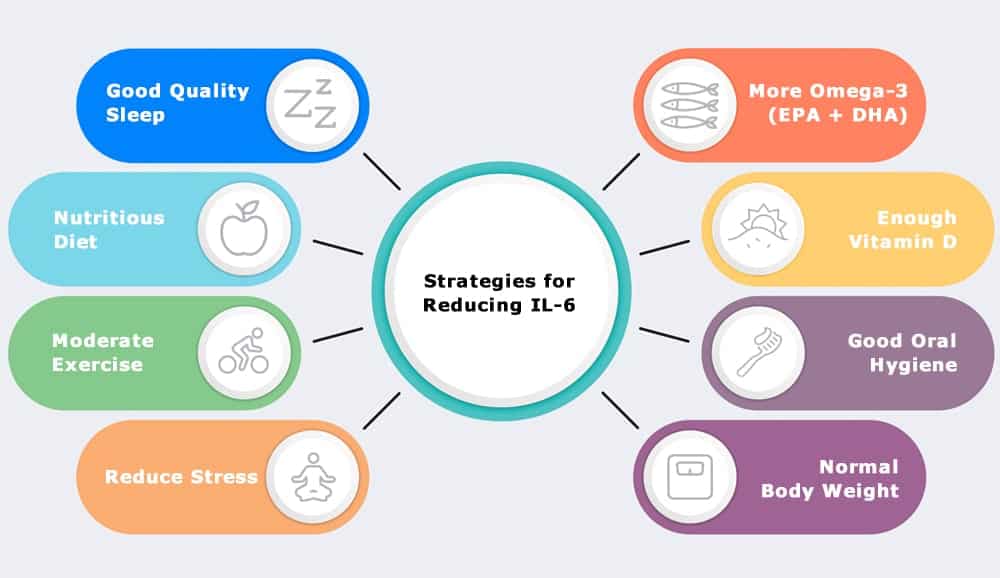
8 Ways to Help Decrease Interleukin-6 Levels
As mentioned above, almost all pro-inflammatory conditions are characterized by increased IL-6. So is there a notable way to reduce interleukin-6 levels?
Certain medical drugs can help for specific conditions like rheumatoid arthritis. However, many common wellness strategies can also make a significant difference. Below are some of the best researched strategies known at this time:
1. Getting Good Quality Sleep
It’s no surprise that getting a good night’s rest is important for maintaining normal IL-6 levels. A meta-analysis of 72 studies found that sleep disturbances were associated with higher IL-6 levels (9). Why? For one, sleeping poorly is typically related with lower melatonin production.
A sizable body of research has separately documented that melatonin supplementation can reduce IL-6 (likely because of melatonin’s anti-inflammatory effect) (10, 11, 12, 13). Indeed, some researchers found that IL-6 levels dropped with as much as 34% after high dose melatonin supplementation (14).
2. Eating a Nutrient-Dense Diet
Eating fast foods made with processed ingredients and loaded with sugar is associated with high IL-6 (15). On the other hand, studies show that people who adhere to a Mediterranean diet – rich in fibers and polyphenols from nuts, legumes, fruits and vegetables – typically have lower IL-6 levels (16).
Consuming enough probiotics also seems to have a significant beneficial effect (4). The same goes for eating more seafood (15).

Eating a Mediterranean Diet – filled with foods rich in fibers, probiotics, polyphenols (antioxidants) and omega-3s – is a great way to reduce IL-6 levels.
3. Getting Enough Vitamin D
The research surrounding vitamin D and IL-6 is not always straightforward. Some meta-analyses have found that vitamin D3 supplementation significantly reduced IL-6 levels (17), while others did not find a similarly significant effect (4).
One thing we do know, however, is that a vitamin D deficiency is associated with increased IL-6 for numerous conditions, so there does seem to be a connection between vitamin D and inflammation (18, 19).
4. Practicing Good Oral Health
Oral hygiene doesn’t often make the typical list of lifestyle recommendations, but there’s good reason to consider it: The mouth is one of the key entry points in the body for bacteria, and therefore, plays a surprising role in the development of disease (20).
Higher IL-6 levels are typically documented in patients with oral health issues like periodontitis, gingivitis, and cavities (even in young children) (21, 22). To date, studies have found that practicing good oral hygiene can help lower the levels of IL-6 again (22).

While IL-6 levels typically spike immediately after exercise, studies show that being active regularly can help decrease IL-6 over time.
5. Moderate Exercise
It’s important for the body to generate enough IL-6 for the right occasions. After exercise, for instance, the body typically produces more IL-6 to help maintain energy and repair any skeletal muscle damage. This is generally a positive thing (23).
The key thing to remember is that, while acute spikes in IL-6 is normal, having chronically high levels becomes problematic. Research shows that those who are less physically active have higher IL-6 levels than disciplined exercisers (16). In addition, researchers have also found that regular exercise, combined with eating a low calorie diet, significantly decreases IL-6 levels (16).
6. Maintaining Normal Body Weight
Obesity is not only associated with chronic, low-grade inflammation – it also seems to fuel it. Our fat tissue increases the production of IL-6, as well as other pro-inflammatory cytokines (24). Conversely, anorexia and other eating disorders are also associated with increased IL-6 levels, so it’s vital to have a healthy approach to weight management (25).

7. Reducing Stress
Stress triggers the release of proinflammatory cytokines (26), so it’s not surprising that people who regularly experience anxiety, fear – or even anger – tend to have higher IL-6 levels (27, 28). These levels also seem to be heightened in people who face regular stressors such as discrimination, and in those who have experienced childhood abuse (29, 30).
While the stressors in our lives are not always within our control, research indicates that there are ways to mitigate the damage. For instance, one study of breast cancer survivors demonstrated that practicing a type of mindfulness therapy (MBSR) helped reduce IL-6 levels (31). That is especially encouraging, since breast cancer survivors frequently continue to struggle with stress and anxiety symptoms after traditional cancer treatment.

When it comes to omega-3s, getting an effective dose matters. Studies show most people need at least 2000 mg of EPA/DHA daily to see an effect on pro-inflammatory markers – and possibly more for obese individuals.
8. Getting Enough Omega-3s
As mentioned above, eating more seafood is associated with lower IL-6 levels. In addition, numerous studies and meta-analyses show that taking omega-3 supplements consistently helps reduce IL-6 levels too. Consider one 2018 study, which found that over the course of 8 weeks, a daily dose of 2500 mg of EPA/DHA reduced IL-6 levels by 22% (32).
Omega-3 supplementation appears to be so effective for reducing IL-6 (and other pro-inflammatory markers) that three recent systematic reviews called it “one of the most promising treatments targeting inflammation in older adults” (4).
Getting an effective omega-3 dose, however, makes a crucial difference. Studies have found that people typically need more than 2000 mg of EPA/DHA per day to reduce the production of proinflammatory interleukins, like IL-6. In addition, higher EPA+DHA doses may be necessary to ultimately reduce levels of proinflammatory interleukins in obese individuals (compared to non-obese individuals) (32).
Omega Restore for Health and Wellness
As a physician-owned and -operated company, Omega3 Innovations has been at the forefront for providing fresh, effectively dosed omega-3 supplements to our customers for more than a decade.
We’ve long understood the synergistic benefits of omega-3 fish oil, melatonin, and vitamin D3 – all key players in reducing interleukin-6 production. This synergy is precisely why we’ve developed Omega Restore – a combination of 3000 mg of EPA/DHA omega-3s with melatonin and vitamin D3.
While there isn’t a single panacea to reduce IL-6 levels, this is a phenomenal way to start improving your quality of health.
For More Restful Sleep and Energy
Experience the Omega3 Innovations difference for yourself with the most effective fish oil supplement on the market.
Buy Now
- Robertson, S. (2020, May 3). “Stratify-and Shield”: A Potential Alternative to COVID-19 Lockdowns. News-Medical.Net.
- Fisman, E. Z., Tenenbaum, A. (2010). The Ubiquitous Interleukin-6: A Time for Reappraisal. Cardiovascular Diabetology, 9 (62).
- Velazquez-Salinas, L., Verdugo-Rodriguez, A., Rodriguez, L. L., & Borca, M. V. (2019). The Role of Interleukin 6 During Viral Infections. Frontiers in Microbiology, 10, 1057.
- Custodero, C., Mankowski, R.T., Lee, S.A., et al. (2018). Evidence-Based Nutritional and Pharmacological Interventions Targeting Chronic Low-Grade Inflammation in Middle-Age and Older Adults: A Systematic Review and Meta-Analysis. Ageing Research Reviews, 46: 42‐59.
- Zhang, X., Tan, Y., Ling, Y. et al. (2020). Viral and Host Factors Related to the Clinical Outcome of COVID-19. Nature.
- Al-Sadi, R., Ye, D., Boivin, M., Guo, S., Hashimi, M., Ereifej, L., & Ma, T. Y. (2014). Interleukin-6 Modulation of Intestinal Epithelial Tight Junction Permeability Is Mediated by JNK Pathway Activation of Claudin-2 Gene. PloS One, 9(3): e85345.
- Liu, F., Lee, S. A., Riordan, S. M., Zhang, L., & Zhu, L. (2019). Effects of Anti-Cytokine Antibodies on Gut Barrier Function. Mediators of Inflammation, 2019, 7028253.
- Copeland, S. H., Warren, S., Lowry, S. F., Calvano, S. E. & Remick, D. (2005). Acute Inflammatory Response to Endotoxin in Mice and Humans. Clinical and Vaccine Immunology, 12 (1): 60-67.
- Irwin, M. R., Olmstead, R., & Carroll, J. E. (2016). Sleep Disturbance, Sleep Duration, and Inflammation: A Systematic Review and Meta-Analysis of Cohort Studies and Experimental Sleep Deprivation. Biological Psychiatry, 80(1): 40–52.
- Zarezadeh, M., Khorshidi, M., Emami, M., et al. (2019). Melatonin Supplementation and Pro-Inflammatory Mediators: A Systematic Review and Meta-Analysis of Clinical Trials. European Journal of Nutrition.
- Yaşar, N. F., Badak, B., Canik, A., Baş, S. Ş., Uslu, S., Öner, S., & Ateş, E. (2017). Effects of Sleep Quality on Melatonin Levels and Inflammatory Response after Major Abdominal Surgery in an Intensive Care Unit. Molecules (Basel, Switzerland), 22(9): 1537.
- Bazyar, H., Gholinezhad, H., Moradi, L., et al. (2019). The Effects of Melatonin Supplementation in Adjunct with Non-Surgical Periodontal Therapy on Periodontal Status, Serum Melatonin and Inflammatory Markers in Type 2 Diabetes Mellitus Patients with Chronic Periodontitis: A Double-Blind, Placebo-Controlled Trial. Inflammopharmacology, 27(1): 67‐76.
- Alamdari, M. N., Mahdavi, R., Roshanravan, N., Yaghin, L. N., Ostadrahimi, A. R. & Faramarzi, E. (2015). A Double-Blind, Placebo-Controlled Trial Related to the Effects of Melatonin on Oxidative Stress and Inflammatory Parameters of Obese Women. Hormone and Metabolic Research, 47(7): 504‐508.
- Sánchez-López, A.L., Ortiz, G.G., Pacheco-Moises, F.P., et al. (2018). Efficacy of Melatonin on Serum Pro-inflammatory Cytokines and Oxidative Stress Markers in Relapsing Remitting Multiple Sclerosis. Archives of Medical Research, 49(6): 391‐398.
- Yeo, R., Yoon, S. R., & Kim, O. Y. (2017). The Association between Food Group Consumption Patterns and Early Metabolic Syndrome Risk in Non-Diabetic Healthy People. Clinical Nutrition Research, 6(3): 172–182.
- Maggio, M., Guralnik, J. M., Longo, D. L., & Ferrucci, L. (2006). Interleukin-6 in Aging and Chronic Disease: A Magnificent Pathway. The Journals of Gerontology, 61(6): 575–584.
- Wang, Y., Yang, S., Zhou, Q., Zhang, H., & Yi, B. (2019). Effects of Vitamin D Supplementation on Renal Function, Inflammation and Glycemic Control in Patients with Diabetic Nephropathy: A Systematic Review and Meta-Analysis. Kidney & Blood Pressure Research, 44(1): 72‐87.
- Manion, M. et al. (2017). Vitamin D Deficiency Is Associated with IL-6 Levels and Monocyte Activation in HIV-Infected Persons. PloS One, 12(5): e0175517.
- Kubesch, A. et al. (2018). Vitamin D Deficiency Is Associated with Hepatic Decompensation and Inflammation in Patients with Liver Cirrhosis: A Prospective Cohort Study. PloS One, 13(11): e0207162.
- Srivastava, M. C., Srivastava, R., Verma, P. K., & Gautam, A. (2019). Metabolic Syndrome and Periodontal Disease: An Overview for Physicians. Journal of Family Medicine and Primary Care, 8(11): 3492–3495.
- Nibali, L., Fedele, S., Donos, N., & D’Aiuto, F. (2013). The Role of Interleukin-6 in Oral Diseases. Dimensions of Dental Hygiene.
- Menon, M. M., Balagopal, R. V., Sajitha, K., Parvathy, K., Sangeetha, G. B., Arun, X. M., & Sureshkumar, J. (2016). Evaluation of Salivary Interleukin-6 in Children with Early Childhood Caries After Treatment. Contemporary Clinical Dentistry, 7(2): 198–202.
- Hennigar, S. R., McClung, J. P., & Pasiakos, S. M. (2017). Nutritional Interventions and the IL-6 Response to Exercise. The FASEB Journal, 31(9): 3719-3728.
- Eder, K., Baffy, N., Falus, A., & Fulop, A. K. (2009). The Major Inflammatory Mediator Interleukin-6 and Obesity. Inflammation Research, 58(11): 727‐736.
- Airov, T. (2018). Elevated Proinflammatory Cytokines Seen in Anorexia Nervosa. Psychiatry and Human Behavioral Health Learning Network.
- Jankord, R., Zhang, R., Flak, J. N., Solomon, M. B., Albertz, J., & Herman, J. P. (2010). Stress Activation of IL-6 Neurons in the Hypothalamus. American Journal of Physiology. Regulatory, Integrative and Comparative Physiology, 299(1): R343–R351.
- O’Donovan, A., Hughes, B. M., Slavich, G. M., Lynch, L., Cronin, M. T., O’Farrelly, C., & Malone, K. M. (2010). Clinical Anxiety, Cortisol and Interleukin-6: Evidence for Specificity in Emotion-Biology Relationships. Brain, Behavior, and Immunity, 24(7): 1074–1077.
- Puterman, E., Epel, E. S., O’Donovan, A., Prather, A. A., Aschbacher, K., & Dhabhar, F. S. (2014). Anger Is Associated with Increased IL-6 Stress Reactivity in Women, But Only Among Those Low in Social Support. International Journal of Behavioral Medicine, 21(6): 936–945.
- Ong, A. D., & Williams, D. R. (2019). Lifetime Discrimination, Global Sleep Quality, and Inflammation Burden in a Multiethnic Sample of Middle-Aged Adults. Cultural Diversity & Ethnic Minority Psychology, 25(1): 82–90.
- Carpenter, L. L., Gawuga, C. E., Tyrka, A. R., Lee, J. K., Anderson, G. M., & Price, L. H. (2010). Association Between Plasma IL-6 Response to Acute Stress and Early-Life Adversity in Healthy Adults. Neuropsychopharmacology: Official Publication of the American College of Neuropsychopharmacology, 35(13): 2617–2623.
- Lengacher, C. A., et al. (2019). A Large Randomized Trial: Effects of Mindfulness-Based Stress Reduction (MBSR) for Breast Cancer (BC) Survivors on Salivary Cortisol and IL-6. Biological Research for Nursing, 21(1): 39–49.
- Tan, A., Sullenbarger, B., Prakash, R., & McDaniel, J. C. (2018). Supplementation with Eicosapentaenoic Acid and Docosahexaenoic Acid Reduces High Levels of Circulating Proinflammatory Cytokines in Aging Adults: A Randomized, Controlled Study. Prostaglandins, Leukotrienes, and Essential Fatty Acids, 132: 23–29.
Popular posts


Related posts