Is It Safe to Take Fish Oil Before Surgery & Medical Procedures?
For years, doctors have advised patients undergoing surgery to stop taking fish oil before their procedure. Because omega-3 fish oil and cod liver oils have a noted blood thinning effect, it was long believed that consuming these kinds of oils could increase a patient’s risk of bleeding during an operation.
New studies, however, have documented that fish oil supplementation before operations not only appears to be safe, but may even be highly beneficial.
So what does that mean for patients and their recovery? Do they really need to stop taking fish oil before surgery?
Is Fish Oil Before Surgery Really a Risk?
The efforts to analyze the hypothetical bleeding risk of omega-3s have been ongoing for years. In 2007, Dr. William Harris, PhD (co-inventor of the omega-3 index) reviewed 19 clinical studies involving more than 4,000 surgical patients. These patients took fish oil supplements at doses ranging from 1.6 to 21g of EPA/DHA per day. In the studies analyzed, the patients also took aspirin or heparin — two common blood-thinning drugs.
The review concluded that the risk of problematic bleeding after taking omega-3 polyunsaturated fatty acids was virtually nonexistent, even when combined with other medications known to increase the risk of bleeding [1].
Another review from 2008 similarly found that no published studies had reported clinically significant bleeding episodes among patients treated with antiplatelet drugs and fish oil at daily doses ranging from 3 – 7g (2).
Omega-3 Fatty Acids Considered Safe
More recent studies have added to the evidence that fish oil supplementation doesn’t increase bleeding risk. One review from 2018 found it safe to consume doses of up to 10g of EPA/DHA per day in the short-term (3). For context, that would be the same as swallowing almost ¼ cup of Omega Cure® fish oil, or taking 33 regular fish oil capsules daily, which is significantly more omega-3 than any patient needs to take.
Similarly, another 2017 study focused on children, also declared that fish oil therapy surrounding surgery was safe and did not increase the risk of bleeding (4).
The takeaway: There’s little evidence to support the need to stop an omega-3 regimen before surgery. On the flip side, fish oil could have benefits for patients before and after operations.
Benefits of Fish Oil Supplements Before and After Surgery
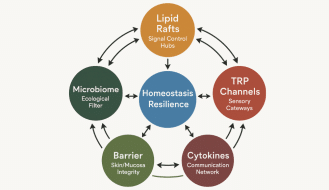
In the medical community today, there’s excitement that omega-3 fatty acids may actually reduce the risk of infections and complications post-surgery. In addition, studies indicate that omega-3s could potentially improve microbiome health, regulate constipation, ease anxiety, and reduce the need for excessive painkillers – all common concerns for surgical patients.
1. Fewer Post-Surgical Infections
One review analyzed the effect of fish oil on pre- and post-surgery colon cancer patients. These types of operations are especially risky due to the high occurrence of postoperative infections. The authors found that omega-3 supplementation was associated with fewer post-surgical infections, as well as a shorter hospital stay (5).
2. Reduced Risk of Cardiac Complications
In a 2017 review, another group of researchers similarly discovered that omega-3 supplementation reduced the length of hospital stays, as well as the risk of atrial fibrillation (6).
A 2018 study co-authored by Dr. William Harris also investigated the risk of bleeding during cardiac surgeries. During the week before their scheduled surgeries, more than 1500 patients were randomly assigned to take either a placebo or 6.5 to 8g of EPA/DHA. Starting from the day of their surgery until their release from hospital, the fish oil group continued to take 1.7g of EPA/DHA.
The results? The team discovered that patients with higher EPA/DHA blood levels actually had a lower risk of bleeding and saw a reduction in the number of blood transfusions (7).
3. Improved Microbial Health
In recent years, researchers have also started to look at the microbiome’s influence on the immune system. The microbiome — the name used to describe the bacteria that live in and on us — can either support or hurt our health, depending on the composition and types of germs.
During surgery, patients are typically both exposed to new types of bacteria and are also given antibiotics that kill off many existing microbial team-players. Both of these factors can disrupt the microbiome, which is why it is important to help support the good bacteria as best as possible.
Studies show that omega-3 fatty acids improve the ratio of beneficial to harmful bacteria, as well as diminish the ability of harmful bacteria to colonize the stomach (8, 9). In addition, fish oil also diminishes the amount of pro-inflammatory endotoxins produced by harmful bacteria (10). All of these benefits can potentially make a big difference for patients’ vulnerable immune systems in a hospital setting.
The research surrounding the microbiome is changing our understanding of disease prevention today. While many factors contribute to microbial health, the types of nutrients we consume — including omega-3 fatty acids — make a big difference.
4. Regulating Post-Surgery Constipation
Studies also suggest that omega-3 fish oil supplementation may be useful in avoiding one of the biggest post-surgical complications: constipation.
Regaining intestinal tract function after surgery can be difficult due to pain medication (especially opioids), diuretics, muscle relaxants, anesthesia, and lengthy bed rest. Using fish oil before surgery, however, can help to lubricate the intestinal tract, allowing for easier bowel movements.
Dr. William Kennedy – a leading US orthopedic surgeon – explains that constipation often results in rising body temperatures, leading many overseeing physicians to believe that their patient is experiencing an infection. In this situation, patients are often prescribed unnecessary antibiotics when a bowel movement could be the simplest solution.
5. Eased Effects of Anxiety
Prior to surgery, it’s common to feel increased anxiety and fear, and more research suggests that fish oil supplements can help manage some of the emotional stress.
In a 2018 meta-analysis, researchers demonstrated a connection between omega-3s and lowered anxiety in patients with a clinical diagnosis — with the caveat that the patients needed an effective omega-3 dose to get results (11).
Further studies also suggests that omega-3s can be beneficial when coping with other instances of stress, like having an acute myocardial infarction, post traumatic stress disorder (PTSD), or even a stressful exam (11). While more clinical studies need to be done with larger sample sizes, these initial findings are promising.
6. Managing Pain and Inflammation
Recovering from surgery is typically a long and painful process, even under the best conditions. But when a person does not get enough omega-3s, they may be putting themselves at risk for extending that process.
Having a high omega-6 to omega-3 ratio is strongly associated with chronic inflammation and pain (12, 13). Furthermore, studies indicate that when patients receive a sufficient daily dose of omega-3 fish oil, it tends to limit their need for painkillers.
Support Your Health with Fresh Fish Oil
It’s time to rethink the old approach of stopping fish oil before surgery. Nobody tells patients to stop eating fish. And as the above research demonstrates, consuming omega-3s from fish oil prior to surgery is similarly safe, unless a person has a bleeding disorder or is on lots of blood thinning medications. In addition, data suggests that getting an effective omega-3 dose can make a difference on you road to recovery.
For patients and practitioners thinking about omega-3 supplementation, however, it is crucial to consider the dose and quality of the oil. For more on that, read “Fresh Fish Oil: Why It Matters to Your Health.”
An Effective Omega-3 Dose, Made Simple
Experience the Omega3 Innovations difference for yourself with the most effective fish oil supplement on the market.
Buy Now
- Harris, W.S. (2007). Expert Opinion: Omega-3 fatty acids and bleeding—Cause for concern? Report of the National Lipid Association’s Safety Task Force: The Nonstatins. American Journal of Cardiology, 99.6A: 44C-6C.
- Braun, L. (2013). Fish Oils and Bleeding: ‘Is There a Clinically Significant Risk? BioCeuticals.
- Jeansen, S., Witkamp, R.F., Garthoff, J.A., van Helvoort, A., and Calder, P.C. (2018). Fish Oil LC-PUFAs Do Not Affect Blood Coagulation Parameters and Bleeding Manifestations: Analysis of 8 Clinical Studies with Selected Patient Groups on Omega-3-Enriched Medical Nutrition. Clinical Nutrition, 37(3):948-957.
- Nandivada, P. et al. (2017). Risk of Post-Procedural Bleeding in Children on Intravenous Fish Oil. American Journal of Surgery, 214(4):733-737.
- Xie, H., and Chang, Y. (2016). Omega-3 Polyunsaturated Fatty Acids in the Prevention of Postoperative Complications in Colorectal Cancer: A Meta-Analysis. OncoTargets and Therapy, 9: 7435–7443.
- Langlois, P.L., Hardy, G., and Manzanares, W. (2017). Omega-3 Polyunsaturated Fatty Acids in Cardiac Surgery Patients: An Updated Systematic Review and Meta-Analysis. Clinical Nutrition, 36(3):737-746.
- Akintoye, E., Sethi, P., Harris, W.S., et al. (2018). Fish Oil and Perioperative Bleeding. Circulation: Cardiovascular Quality and Outcomes, 11(11):e004584.
- Correia, M. et al. (2012). Docosahexaenoic Acid Inhibits Helicobacter Pylori Growth In Vitro and Mice Gastric Mucosa Colonization. PloS One, 7(4), e35072.
- Kim, Y. G., Lee, J. H., Raorane, C. J., Oh, S. T., Park, J. G., and Lee, J. (2018). Herring Oil and Omega Fatty Acids Inhibit Staphylococcus aureus Biofilm Formation and Virulence. Frontiers in Microbiology, 9, 1241.
- Kaliannan, K. et al. (2015). A Host-Microbiome Interaction Mediates the Opposing Effects of Omega-6 and Omega-3 Fatty Acids on Metabolic Endotoxemia. Scientific Reports, 5, 11276.
- Su, K. P., Tseng, P. T., Lin, P. Y., Okubo, R., Chen, T. Y., Chen, Y. W., and Matsuoka, Y. J. (2018). Association of Use of Omega-3 Polyunsaturated Fatty Acids With Changes in Severity of Anxiety Symptoms: A Systematic Review and Meta-Analysis. JAMA Network Open, 1(5), e182327.
- Sibille, K. T. et al. (2018). Omega-6: Omega-3 PUFA Ratio, Pain, Functioning, and Distress in Adults With Knee Pain. The Clinical Journal of Pain, 34(2), 182–189.
- DiNicolantonio, J. J., and O’Keefe, J. H. (2018). Importance of Maintaining a Low Omega-6/Omega-3 Ratio for Reducing Inflammation. Open Heart, 5(2), e000946.
Popular posts


Related posts