Omega-3s Are Good for the Heart, According to Landmark Meta-Analysis
Can omega-3s prevent heart disease? That’s been one of the key questions in nutrition since Danish researchers Dyerberg and Bang published their first study on omega-3 fatty acids in the early 1970s.
Over the following 50 years, the role of omega-3s in heart health has generated an enormous body of research. While earlier studies found significant promise, more recent trials suggested that omega-3 supplements offered few heart health benefits.
Now, new research published in Mayo Clinic Proceedings solidifies a message we’ve been asserting for years: Omega-3 benefits are dose dependent, and how much we consume can make the difference between zero results and lifesaving outcomes.
Can Omega-3s Prevent Heart Disease?
In September 2020, an authoritative meta-analysis published in the journal Mayo Clinic Proceedings presented some stunning findings. Taking effective doses of omega-3s was associated with:
• A 35% reduced risk of having a fatal heart attack.
• A 13% reduced risk of having a heart attack.
• A 10% reduced risk of having a coronary heart disease event.
• A 9% reduced risk of dying from coronary heart disease (1, 2).
The researchers also concluded that these benefits likely depended on the dose consumed. For instance, there was an additional 9% reduction in heart attack risk with each additional 1000 mg of EPA/DHA consumed daily.
What Does Previous Heart Disease Research Say?
The news from Mayo Clinic Proceedings is not terribly surprising for those of us who have followed omega-3 research for years. Already in 2008, The Wall Street Journal highlighted the discrepancy between omega-3 doses used in successful clinical trials and the doses most Americans were (and still are) consuming (3).
In 2012, we at Omega3 Innovations similarly made a video addressing the importance of getting enough omega-3s in order to experience benefits. Since that time, this video has been watched over 140,000 times.
The point is that scientists have known for a long time that there is a strong relationship between omega-3 dose and benefits. Research has consistently demonstrated that effective doses of omega-3s can reduce elevated triglyceride levels and high blood pressure – two common risk factors for heart disease (4, 5, 6).
Other cardiovascular issues – like arrhythmia and atherosclerosis (the buildup of arterial plaque) – also seem to be helped by higher doses of omega-3s. A 2020 review from Saint Luke’s Mid America Heart Institute concluded that omega-3s exhibit antiarrhythmic effects, with daily doses of 3000 mg of EPA/DHA and up having the greatest impact (7). Similarly, a 2019 meta-analysis also found that taking 3000 mg of EPA/DHA (or more) significantly slowed the progression of atherosclerosis (8).
Numerous studies have additionally shown that higher omega-3 index levels are associated with a lower risk of fatal coronary heart disease and sudden cardiac arrest (9, 10, 11).
Past Clinical Studies Likely Failed Because of Low Doses
In contrast to the aforementioned studies, clinical trials using lower daily doses of omega-3s (1000 mg of EPA/DHA or less) typically never find good results. In fact, between 2010 and 2018, a series of omega-3 studies that used low doses all concluded that fish oil supplements had little to no effect on heart disease (12, 13).
These studies threw doubt on the cardiovascular benefits of omega-3s as a whole. To some extent, this critique was warranted, given that these clinical trials better reflected the small doses most Americans were consuming (around 300 mg of EPA/DHA per capsule).
The 2020 findings from Mayo Clinic Proceedings support the conclusion that previous heart health studies likely failed due to low doses. Their findings have even prompted GOED (the main trade organization for omega-3 manufacturers) to rethink their current omega-3 recommendations in favor of higher doses (2).
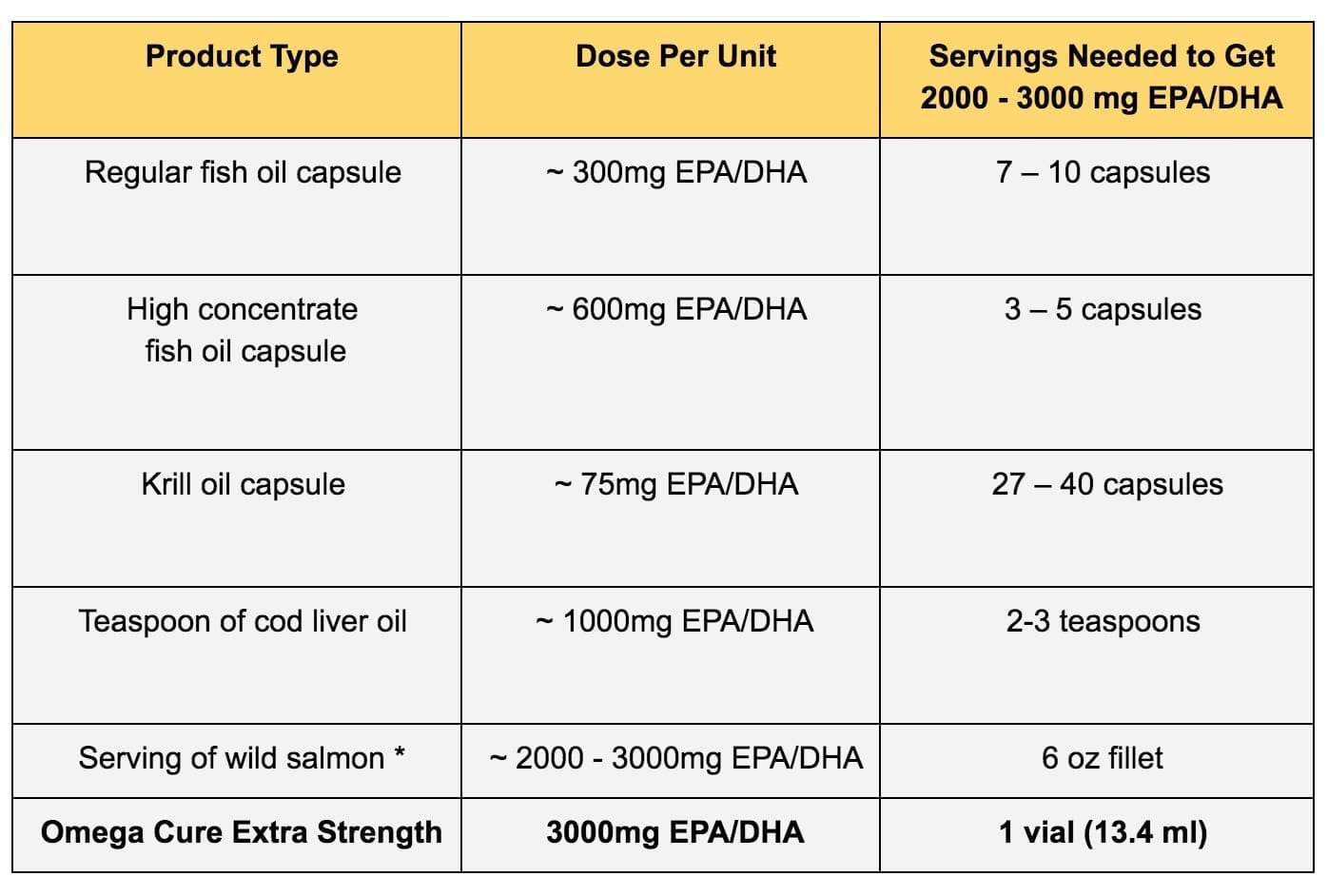
* The omega-3 content of a serving of salmon can vary depending on factors like the fish species, how it was prepared, etc. Still, eating fatty fish, like salmon, vastly outperforms regular fish oil capsules in terms of dose.
How Much Omega-3 Do We Need for Good Heart Health?
In the Mayo Clinic Proceedings meta-analysis, the researchers recommended taking between 1000 – 2000 mg of EPA/DHA per day. That said, other researchers frequently cite higher doses (≥ 2000 mg of EPA/DHA and ≥ 3000 mg of EPA/DHA) for patients with conditions such as:
• Elevated triglyceride levels
• Anxiety
• Cancers, and more.
Higher Doses May Deliver Even Better Results
While getting 1000 – 2000 mg of EPA/DHA daily may elicit some heart health protection, it is also likely that taking higher omega-3 doses may provide greater effects. The Mayo Clinic Proceedings meta-analysis alluded to this phenomenon by showing that the risk of having a heart attack falls by an additional 9% for every 1000 mg of EPA/DHA consumed – and they are not the first to document this trend.
Consider another 2020 review from researchers at the University of Oslo. When comparing past omega-3 trials, they found a strong relationship between omega-3 dose and the relative impact on triglyceride levels (12). The pattern is striking:
• In one study, 850 mg of EPA/DHA reduced triglyceride levels by only 3.4%.
• In a later study, 2400 mg of EPA/DHA reduced triglyceride levels by 16%.
• In a third study, 5100 mg of EPA/DHA dropped triglyceride levels by 27%.
The relationship between dose and benefits can also be seen in comparative blood samples. For instance, one 2018 study analyzed the omega-3 index levels of Japanese men. Those with omega-3 index levels of 10% or higher had a statistically greater reduction in cardiovascular disease risk, compared to men with omega-3 index levels of 8% (9).
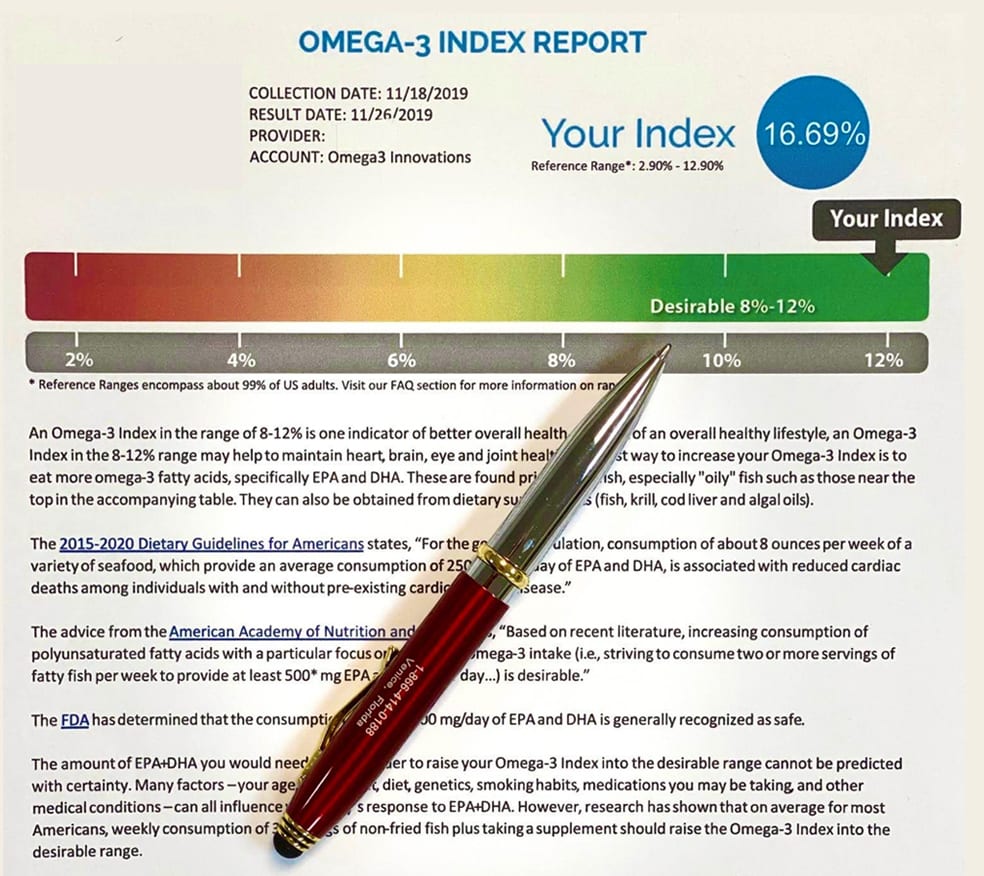
The omega-3 index measures how much EPA and DHA is found in a person’s red blood cells. While most Americans have low omega-3 index levels under 4%, it’s considered best to have levels above 8% .
Dose May Also Depend on Diet & Health
Hopefully, future research will further clarify what constitutes an effective omega-3 dose. Very likely, the answer will depend – at least in part – on the individual. For instance, we know that most Americans need significantly more omega-3s to achieve clinical benefits compared to, say, the Japanese. That’s because, as a group, the Japanese eat significantly more seafood than Americans, highlighting the role of diet in the dosage equation (8).
Scientists also suspect that people who struggle with health issues, like obesity, may need higher omega-3 doses as well (14).
Fortunately today, people can take a simple blood test to assess their omega-3 needs. With all of the individual variations, such personalized information can help consumers make informed decisions about the best omega-3 dose for them.
Omega-3 Dose Isn’t the Only Thing That Matters
As the research shows, getting an effective EPA/DHA dose is critical for obtaining omega-3 benefits. However, it’s important to remember that three additional points also play a key role in determining health outcomes:
1. Make Sure Your Omega-3 Supplement Is Fresh
You’d never eat old fish for dinner, so why would you take a rancid omega-3 supplement?
Fresh fish doesn’t taste or smell fishy, and neither does fresh fish oil. Only when an omega-3 product starts to spoil (or oxidize) does it acquire a strong fishy taste and smell. While many manufacturers put fish oil into capsules, this only conceals the problem.
Getting fresh omega-3 fish oil is critical for both safety and efficacy reasons. While an omega-3 oil should ideally have a peroxide value below 2 mEq/kg, many fish oils exceed 5 mEq/kg at the time of consumption (15, 16). In comparison, Omega Cure® typically has a peroxide value ranging from 0.1 – 0.5 mEq/kg, which explains why it doesn’t have a fishy taste or smell. We’re even able to use the oil to make high-dose omega-3 cookies and chocolates.
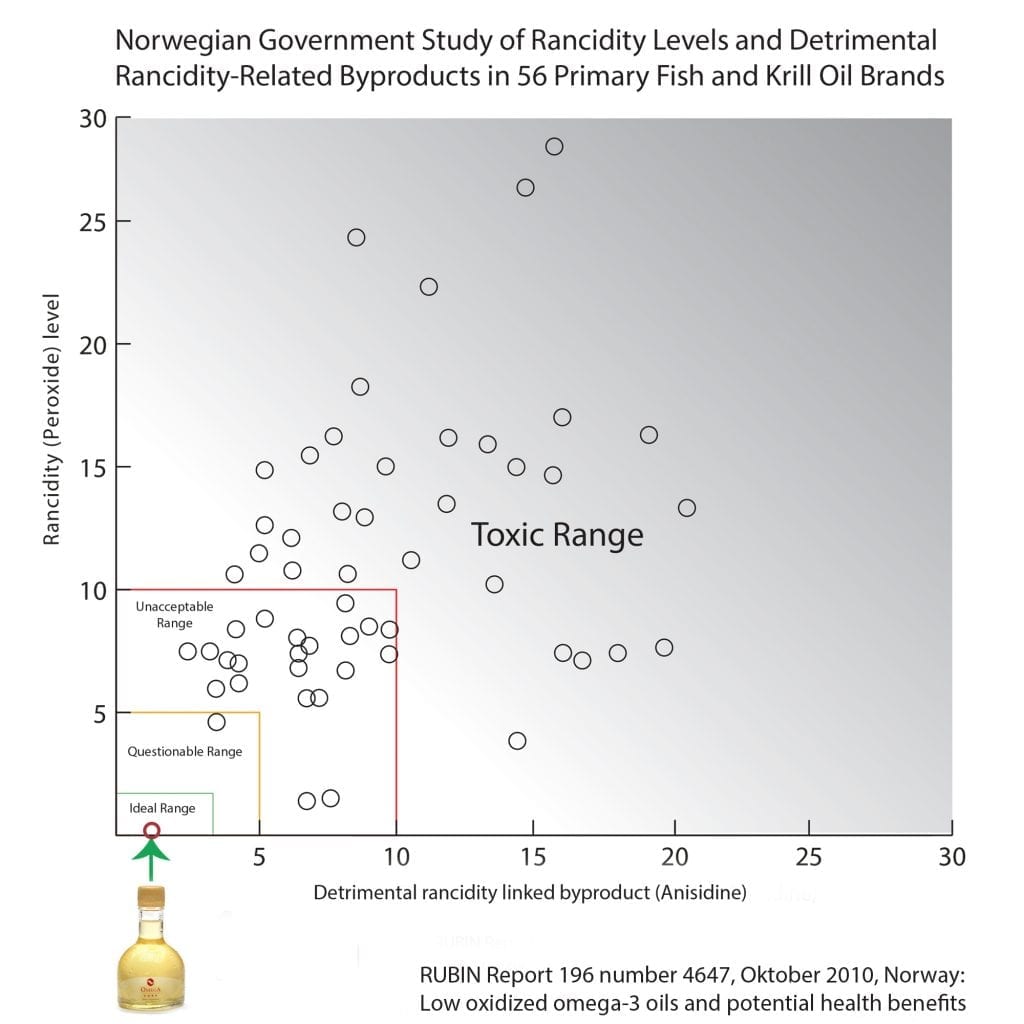
The results from one independent 2010 analysis of omega-3 products in Norway. It included our Omega Cure cod liver oil.
2. Consider Liquid Fish Oil Over Capsules
Why did earlier omega-3 studies find greater benefits than later trials? While many factors likely influenced the outcomes, we speculate that older studies found superior results due to the fact that they used liquid cod liver oil.
Cod liver oil – one of nature’s oldest and best sources of omega-3s – was normally taken by the spoonful, not as a pill. As we’ve covered previously, liquid omega-3 products have numerous benefits compared to capsules, particularly with regard to dose and influence on the microbiome.
3. Get the Full Range of Omega-3 Fatty Acids
Over the years, pharmaceutical companies (and many omega-3 manufacturers) have increasingly moved towards creating highly processed, patentable formulations of “EPA-only” and “DHA-only” products. This trend has led some people to wonder about the optimal ratio of these fatty acids. In the Mayo Clinic Proceedings meta-analysis, the research team said there was not enough data yet to draw conclusions about the relative benefits of EPA-only vs. EPA+DHA supplements.
We’re sure that, in time, research will favor less processed oils that provide effective doses of both EPA and DHA. After all, each member of the omega-3 family has unique and synergistic effects. In addition, they are normally found together in nature. For all of these reasons, we believe it’s important to get the full spectrum of the omega-3 fatty acid family for optimal health.
Sitting down with celebrated orthopedic surgeon Dr. William Kennedy, we discussed the difference between our Omega Cure oil and a frequently-prescribed omega-3 capsule.
Why Omega3 Innovations Is Different
Since we launched Omega3 Innovations in 2006, our approach to omega-3s has been unique. We’ve worked hard to ensure that all of our products deliver effective EPA + DHA doses. Our Omega Passion® chocolates match the Mayo Clinic Proceedings meta-analysis recommendations (with 1500 mg of EPA/DHA per serving), and our Omega Cure Extra Strength and Omega Restore vials deliver 3000 mg of EPA/DHA for adults who need higher doses.
Besides focusing on dose, we resolutely do not make fish oil capsules, we focus on freshness at every stage of production, and we value providing our customers with an extraordinary full-spectrum oil.
As medical doctors, our passion for wellness comes from the heart. If you have questions about the topics covered here, let us know in the comments.
An Effective Omega-3 Dose, Made Simple
Experience the Omega3 Innovations difference for yourself with the most effective fish oil supplement on the market.
Buy Now
References:
1. Bernasconi, A. A., Wiest, M. M., Lavie, C. J., Milani, R. V., Laukkanen, J. A. (2020). Effect of Omega-3 Dosage on Cardiovascular Outcomes: An Updated Meta-Analysis and Meta-Regression of Interventional Trials. Mayo Clinic Proceedings, S0025-6196(20)30985-X.
2. Schultz, H. (2020, September 17). Meta-Analysis Finds Strong Support for Cardiovascular Health Benefits of Omega-3s. NutraIngredients-USA.
3. Stipp, D. (2008, January 8). Fish-Oil Doses Can Be Hard to Swallow. The Wall Street Journal.
4. Tenenbaum, A., & Fisman, E. Z. (2018). Omega-3 Polyunsaturated Fatty Acids Supplementation in Patients with Diabetes and Cardiovascular Disease Risk: Does Dose Really Matter? Cardiovascular Diabetology, 17(1), 119.
5. Miller, P. E., Van Elswyk, M., & Alexander, D. D. (2014). Long-Chain Omega-3 Fatty Acids Eicosapentaenoic Acid and Docosahexaenoic Acid and Blood Pressure: A Meta-Analysis of Randomized Controlled Trials. American Journal of Hypertension, 27(7), 885–896.
6. Skulas-Ray, A. C., Kris-Etherton, P. M., Harris, W. S., & West, S. G. (2012). Effects of Marine-Derived Omega-3 Fatty Acids on Systemic Hemodynamics at Rest and During Stress: A Dose-Response Study. Annals of Behavioral Medicine: A Publication of the Society of Behavioral Medicine, 44(3), 301–308.
7. DiNicolantonio, J. J., & OKeefe, J. (2020). The Benefits of Marine Omega-3s for Preventing Arrhythmias. Open Heart, 7(1), e000904.
8. Sekikawa, A., Cui, C., Sugiyama, D., Fabio, A., Harris, W. S., & Zhang, X. (2019). Effect of High-Dose Marine Omega-3 Fatty Acids on Atherosclerosis: A Systematic Review and Meta-Analysis of Randomized Clinical Trials. Nutrients, 11(11), 2599.
9. Harris, W. S. (2018). Redefining Target Omega-3 Index Levels: The Japan Public Health Center Study. Atherosclerosis, 272, 216-218.
10. Harris, W. S., Del Gobbo, L., & Tintle, N. L. (2017). The Omega-3 Index and Relative Risk for Coronary Heart Disease Mortality: Estimation from 10 Cohort Studies. Atherosclerosis, 262, 51-54.
11. Von Schacky, C. (2010). Omega-3 Index and Sudden Cardiac Death. Nutrients, 2(3), 375–388.
12. Arnesen, H., Myhre, P. L., & Seljeflot, I. (2020). Very Long Chain Marine n-3 Polyunsaturated Fatty Acids in Atherothrombotic Heart Disease. A Brief Review, with a Focus on Metabolic Effects. Nutrients, 12(10), 3014.
13. Schatzker, M., & Bazinet, R. (2018, November 19). Do Fish Oil Supplements Work? Science Keeps Giving Us Slippery Answers. Vox Media.
14. Tan, A., Sullenbarger, B., Prakash, R., & McDaniel, J. C. (2018). Supplementation with Eicosapentaenoic Acid and Docosahexaenoic Acid Reduces High Levels of Circulating Proinflammatory Cytokines in Aging Adults: A Randomized, Controlled Study. Prostaglandins, Leukotrienes, and Essential Fatty Acids, 132: 23–29.
15. Jackowski, S. A., Alvi, A. Z., Mirajkar, A., Imani, Z., Gamalevych, Y., Shaikh, N. A., & Jackowski, G. (2015). Oxidation Levels of North American Over-the-Counter N-3 (Omega-3) Supplements and the Influence of Supplement Formulation and Delivery Form on Evaluating Oxidative Safety. Journal of Nutritional Science, 4, e30.
16. Albert, B. B., Derraik, J. G., Cameron-Smith, D., Hofman, P. L, et al. (2015). Fish oil Supplements in New Zealand are Highly Oxidised and Do Not Meet Label Content of N-3 PUFA. Scientific Reports, 5, 7928.
Popular posts


Related posts